How to Prevent Colorectal Cancer
Between 66% and 75% of colorectal cancer cases can be prevented by having a healthy diet and lifestyle.
Table of contents
- Conclusions
- Is colorectal cancer a matter of genes or lifestyle?
- Our eating habits are the source of most carcinogens
- How a diet based on fruits, vegetables, and spices prevents colorectal cancer
- How to prevent colorectal cancer — key points
- What about genetic predisposition for colorectal cancer?
- Bibliography
Conclusions
Among the many types of cancers, colorectal cancer is one that is most influenced by diet and lifestyle.1
The main factors that cause colorectal cancer are eating meat (especially when it has been cooked and preserved using chemicals), consuming saturated fatty acids, trans fatty acids, refined sugar, and white flour; having long-term exposure to chlorinated drinking water; not getting enough physical activity; and suffering from obesity. Consuming grains and dairy products may be detrimental to colorectal conditions as well, but further and specific research is needed.
A plant-based diet has the potential to prevent and even reverse colorectal cancer because of its high content of phytonutrients and substances which inhibit the "growing" and proliferation of cancer cells.
Foods with a high content of anticancer substances include turmeric (curcuma), garlic, watermelon, apricots, pink guava, grapefruit, rosehip, tomatoes, grapes, peanuts, berries, onions, apples, the dried fruit of the milk thistle plant Silybum marianum, cabbage, broccoli, brussels sprouts, cauliflower, daikon, artichoke, and fenugreek.
Vitamins D and E, folic acid, and calcium have specific protective effects against colorectal cancer.
| Not only vegans and vegetarians should read this: A Vegan Diet Can Be Unhealthy. Nutrition Mistakes. |
Is colorectal cancer a matter of genes or lifestyle?
Approximately 1'235'108 people are diagnosed annually with colorectal cancer, and 609'051 die from it. The World Health Organization estimates an increase of 77 % in the number of newly diagnosed cases of colorectal cancer and an 80 % increase in deaths by 2030.2
Important facts about colorectal cancer
- It is the third most common type of cancer in men and the second most common in women (after breast cancer).
- Most of the colorectal cancer cases occur in developed countries.
- Korea has the highest incidence of colorectal cancer, followed by Slovakia, Hungary, Denmark, and the Netherlands.3
- In Europe, colorectal cancer is the third most common type of cancer and is one of the leading causes of cancer death. Estimates show that every year there is a 0.5 % increase in the incidence of colorectal cancer in European countries.2
Colorectal cancer, colon cancer or rectal cancer? What is the difference?
Most of the times, the terms “colorectal cancer” and “colon cancer” are used interchangeably because anatomically, the rectum represents the last 12 cm (4.7 in) of the colon.
The main differences between colon cancer and rectal cancer are related to the anatomy of the organ, the genetic determination of disease, invasion of the nearby tissues and the surgical approach of the treatment.
However, the risk factors, the possible causes and diet’s impact on this conditions are relatively similar. 27
In his studies, Craig Venter, a pioneer in genomic research, explains the complexity of human biology and how, despite common understanding, genes have very little impact on life outcomes. Genes can provide useful information about the risks of a disease, but in most cases they will not determine the actual cause of the disease, nor its incidence. Life outcomes are determined by environmental factors and the complex interaction between all of the cells in the human body.4
Studies involving identical twins have had similar results, proving that the source of most chronic illnesses can be found in the environment and not in our genes.5
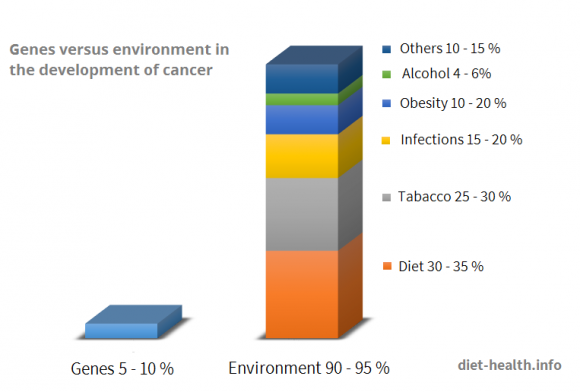
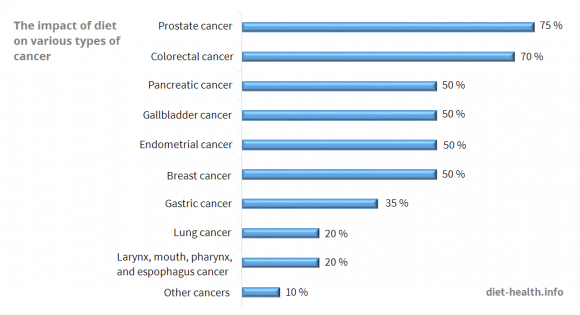
Willett (1995) investigated the correlation between cancer deaths and diet and also determined that colorectal cancer is among the types of cancer most affected by nutrition.6
According to Willett, 75 % of prostate cancer deaths could be avoided by dietary change. The same applies to 70 % of colorectal cancer deaths and 50 % of pancreatic, gallbladder, endometrial, or breast cancer deaths.
Excessive energy intake is thought to be one of the main reasons why diet has such a strong influence on most types of cancer.
Studies on animals have shown that “the impact of energy restriction can be profound — for example, a 30 % lower intake has reduced mammary tumors by as much as 90 %.”6 Even if further research on humans is necessary, this could be a solid starting point in understanding the impact diet has on cancer in general and on colorectal cancer development in particular.
Our eating habits are the source of most carcinogens
The increase in cancer incidence has occurred in parallel with economic development.
Worldwide, the majority of colorectal cancers continue to occur in industrialized countries, although incidence rates are rapidly rising in less-developed nations as they increasingly adopt features of a Western lifestyle.7
The majority of substances we consume that are capable of causing cancer come from food, food additives, and the cooking process:
- When meat is cooked, carcinogenic substances (heterocyclic amines) form.
- Charcoal cooking and curing and smoking meat produces harmful carbon compounds that have a cancerous effect.
- Nitrites and nitrates used for meat preservation are strong carcinogens.7
- Saturated fatty acids, trans fatty acids, refined sugar, and white flour present in many foods have also been associated with digestive cancers.
- Long-term exposure to chlorinated drinking water has been linked to an increased risk of cancer. Nitrates, in drinking water and some foods, can transform to mutagenic N-nitroso compounds, which then increase the risk of lymphoma, leukemia, colorectal cancer, and bladder cancer.9
Eating red meat increases the risk of colorectal cancer
The European Prospective Investigation into Cancer and Nutrition (EPIC), a study conducted on a group of 478'040 people from ten European countries, showed that colorectal cancer is strongly associated with the intake of red meat and processed meat.
After a period of 4.8 years, 1'329 of the 478'040 individuals enrolled in the study had developed colorectal cancer.
After taking into consideration factors such as age, sex, sources of energy, height, weight, physical activity, smoking, dietary fiber, and folate and alcohol consumption, the researchers determined that eating more than 20 g of red and/or processed meat per day is associated with an increased risk of colorectal cancer, and the correlation only becomes stronger when the quantity of red/processed meat surpasses 160 g/day.
Obesity has a direct impact on colorectal cancer
Colorectal cancer is one of the types of cancer that is directly associated with obesity and excess weight.
After 16 years of follow-up, a study10 on 900'000 Americans without cancer registered 57'145 deaths from cancer. Using research models which controlled other risk factors, the study showed that body mass index was significantly associated with higher rates of death from colorectal cancer.
The explanation resides in the activity of NF-κB, a protein involved in DNA transcription, cell survival, and cellular responses to external stimuli. Hyperglycemia and certain substances produced by the fat cells disturb the function of NF-κB, which can then lead to cancer and other immune disorders.
Metabolic syndrome is a risk factor for developing colorectal cancer
Metabolic syndrome represents the expression of at least three of the following medical conditions: increased waist circumference, elevated blood pressure, hyperglycemia, high serum triglycerides, and low high-density lipoprotein (HDL).
Metabolic syndrome in itself or associated with nonalcoholic fatty liver disease represents a significant risk for developing colorectal cancer.11
Milk and dairy products can be detrimental for colorectal conditions
A correlation between the consumption of dairy products and the risk of colorectal cancer has not yet been established. At this stage, information is still contradictory, making it difficult to develop public health recommendations.
In helping to prevent the development of colorectal cancer, the strongest argument in favor of dairy consumption would be the high level of calcium found in milk. On the other hand, more in-depth studies presented here and here show that the human body absorbs very little of the calcium in milk.
Furthermore, dairy consumption may even increase calcium loss in bones, and the ability that calcium in milk has to prevent colorectal cancer is likely canceled out by the high fat content of dairy products.
Although the EPIC Study, one of the broadest studies investigating the association between diet, lifestyle, and various types of cancer, concluded that dairy products may have a protective role when it comes to colorectal cancer, other prospective studies show that, despite their high calcium content, milk and dairy products are detrimental to colorectal conditions.
- In Great Britain, among 5'000 children with a diet high in dairy products, the incidence of colorectal cancers after a 65-year follow-up was three times higher as compared to children from families with a low dairy intake.12
Lack of exercise and a sedentary lifestyle are associated with colorectal cancer
A lack of physical activity has been associated with most chronic illnesses, and in the case of colorectal cancer the impact of a sedentary lifestyle has been demonstrated to be significant.11
A reduction of almost 50 % in the incidence of colon cancer was observed among those with the highest levels of physical activity.13
Here are the main ways physical inactivity facilitates the development of colorectal cancer:
- Sedentarism decreases the intestinal transit. This means that the body stays in contact with potential carcinogens for longer periods of time.
- Inactivity increases the circulating levels of "insulinhormone" in the body, which promotes the multiplication of the epithelial cells in the colon.
- A lack of exercise alters prostaglandin levels. Prostaglandins are hormone-like substances that regulate inflammation and "cellgrowth".
- Sedentarism depresses the immune function, depleting the body from its capacity to fight the proliferation of cancer.
How a diet based on fruits, vegetables, and spices prevents colorectal cancer
Since 1960, numerous scientific studies have shown that eating certain fruits and vegetables regularly may have a protective effect against cancer.
There are more than 25'000 different plant substances (phytochemicals) that have been shown to influence various cancers. The advantage of these phytochemicals is that they are safe and usually influence multiple cell functions simultaneously.
Here are the phytochemicals that have a significant impact on colorectal cancer:
| Phytochemical | Action | Significant Amounts Found In: |
| Diallyl disulfide | Inhibits the "growing" and proliferation of cancer cells in the colon (studies on humans and rats) | Garlic |
| Carotenoids (especially lycopene) | Proven anticancer activity in both in vitro and in vivo tumor models, as well as in humans Help in the detoxification process Interfere with cell proliferation Facilitate communication between cells Inhibit multiplication of cancerous cells | Watermelon, apricots, pink guava, grapefruit, rose hip, and tomatoes |
| Resveratrol | Inhibits "tumorgrowth" Currently, substances with a chemical structure similar to resveratrol are produced as “potential chemo preventive and therapeutic agents for cancer”13 | Grapes, peanuts, and berries |
| Quercetin | Antioxidant and anti-inflammatory effects Stops cell multiplication Regulates the death of old or sick cells Blocks NF-κB activation | Onions and apples |
| Silymarin | Antioxidant and anti-inflammatory effects Protects the liver Could reverse, suppress, or prevent cancer progression (studies on rodents) | The dried fruit of the milk thistle plant Silybum marianum |
| Indole-3-carbinol and Sulforaphane (SFN) | Metabolize and detoxify carcinogens, including estrogens | Cabbage, broccoli, brussels sprouts, cauliflower, daikon, and artichokes |
| Diosgenin | Inhibits cell proliferation Induces the controlled death of cancerous cells Suppresses intestinal inflammation | Fenugreek |
Curcumin, the plant compound with the highest impact on colorectal cancer
Curcumin is the active ingredient in turmeric (ingredient in curry powder) and is also found in smaller quantities in ginger.
Over 3'000 published studies have demonstrated the impact of curcumin on cancer in general, and many studies have also examined its effects on colorectal cancer. Curcumin inhibits inflammation, interacts with a wide variety of proteins and modifies their activity, and has a direct impact on cell survival, proliferation, invasion, and angiogenesis (formation of new blood vessels).
Two of the main research studies on this topic highlight the effects of curcumin on colorectal cancer:
- In a study on patients with familial adenomatous polyposis (cancer of the large intestine and rectum), a treatment with curcumin and quercetin for approximately six months led to a decrease in polyp number and size.7
- A study on patients with advanced colorectal cancer, a daily dose of 3.6 g of curcumin resulted in a 62 % decrease in inducible prostaglandin E2 (substances in the blood that show the degree of inflammation) production on day 1 and a 57 % decrease on day 29.
Dietary fiber has a direct impact on colorectal cancer
Dietary fiber is a plant component found in whole grains, dried beans and peas, as well as fruits and vegetables. It can’t be digested and absorbed by the human body and therefore passes relatively intact through the stomach, small intestine, and colon.
Research studies have shown that fiber influences the development of cancer by:
- diluting potential carcinogens and speeding their transit through the colon,
- binding carcinogenic substances,6
- altering the colonic flora,6
- reducing the pH,6 and
- producing short-chain fatty acids (through fiber fermentation), which are an important suppressor of tumor formation.15
While the impact of fiber on colorectal cancer has been proven to be beneficial, the source of this fiber is still disputed.
Thanks to the fiber, macronutrients, vitamins, and minerals they contain, whole grains are considered to have an important function in preventing colorectal cancer.
Whole grains contain chemo preventive antioxidants such as vitamin E, tocotrienols, phenolic acids, lignans, and phytic acid. The antioxidant content of whole grains is less than that of some berries but is greater than that of common fruits or vegetables.16
Furthermore, it has been determined that whole grains help maintain a stable blood sugar level, which is also important because hyperglycemia is a significant risk factor for colon cancer.17
However, other research studies6 have shown that after taking the combined action of all of the other risk factors into consideration, eating whole grains is not associated with a lower risk of colon cancer.
Moreover, there are even studies supporting the idea that grains could be associated with an increased risk of colon cancer.6
Vitamins and minerals with chemo-preventive action
Various studies regarding the nutritional and environmental factors that have a potential impact on colon cancer emphasize the importance of specific vitamins and minerals in preventing and managing this disease.
Vitamin D
Among all types of cancer, colorectal cancer is the type most influenced by circulating levels of vitamin D. The higher the vitamin D intake, the lower the risk of colorectal cancer.
- The EPIC (European Prospective Investigation into Cancer and Nutrition) study measured vitamin D blood levels for 1'248 subjects diagnosed with colorectal cancer and compared them with the levels measured in a group of noncancer patients with similar characteristics (sex, age, and other relevant variables). The blood vitamin D concentration was inversely correlated with the risk of colorectal cancer in both men and women.
- In a follow-up study that examined survival after the diagnosis of colorectal cancer, subjects with higher blood vitamin D levels at baseline showed significantly longer survival rates.7
Vitamin E
In a number of individual studies, vitamin E supplements were associated with a reduced risk of colon cancer.19
Selenium
The capacity of selenium to reduce the risk of different types of tumors has been shown primarily in animal studies.20 Observational studies on various populations have shown an inverse association between selenium and colon cancers,21 and experimental studies have demonstrated a significant and rapid reduction in the incidence of colon cancer among those receiving selenium supplements.6
Calcium
The beneficial impact of calcium in reducing the risk of colon cancer was first demonstrated in animal studies.
Even if some researchers claim that “a weak or modest impact was registered in human trials,”22 some studies show significant changes in the colon tissue and a significantly reduced risk of colorectal cancer in both men and women who took 2.0 g of calcium daily and/or 800 IU (20 µg) of vitamin D over a period of six months.23
Folic acid
Various studies have associated a lower intake of folic acid with an increased risk of colon cancer, and some reports have demonstrated that the use of multivitamins containing folic acid could lower the risk of colon cancer.23
However, based on the data gathered in the Nurses’ Health Study researchers have shown that although the results of folic acid supplementation are not significant in the first 15 years, the impact is substantial beyond this time (a 75 % lower risk).24
How to prevent colorectal cancer — key points
 | Keep your weight between the recommended limits (BMI 19–25 kg/m2). Do moderate to vigorous physical activity for a minimum of 30 minutes, at least 5 days a week. Consume a diet based on fruits and vegetables. Replace meat and dairy with fish, nuts, and legumes. Consume unsaturated fats. Limit alcohol consumption. Give up smoking. Make sure you have normal levels of folic acid and vitamins D and E. Consume whole grains. Give up processed and refined products. Eat fruits, vegetables, and spices that have a positive influence on digestion. |
What about genetic predisposition for colorectal cancer?
In some situations, colorectal cancer can be inherited. The genetic component of this condition is considered to be strong when:
- there is a long family history of polyps and even colorectal cancer (the presence of two or more first-degree relatives affected by colorectal cancer accounts for more than 20 % of all cases25),
- when family members already have conditions or syndromes considered to increase the risk of colorectal cancer (e.g., endometrial cancer, Lynch syndrome, or familial adenomatous polyposis),
- when colorectal cancer develops at an early age, or
- when the person has an Ashkenazi Jewish background (because of a gene fault that is more common in this group).26
Furthermore, there are other conditions as well which can increase the risk of colorectal cancer: preexisting benign polyps in the bowel, ulcerative colitis and Crohn’s disease, diabetes, acromegaly, gallstones, infections with Helicobacter pylori and Human papilloma virus, and radiation exposure.25
Since genetic testing can identify only a small part of all gene mutations which can lead to colorectal cancer, regular screening tests are necessary.
People with no risk of colorectal cancer should undergo regular screening tests starting at age 50 and repeat these every ten years. People who have an increased risk because of family or personal history, bowel inflammatory diseases, or other inherited conditions should start the screening before age 50 and undergo more frequent tests.
Literature — sources:
27 sources
- Giovannucci E. Modifiable risk factors for colon cancer. Gastroenterol Clin North Am. 2002 Dec;31(4):925-43.
- Binefa G, Rodríguez-Moranta F, Teule À, Medina-Hayas M. Colorectal cancer: From prevention to personalized medicine. World Journal of Gastroenterology : WJG. 2014;20(22):6786-6808.
- Ferlay J, Soerjomataram I, Ervik M, Dikshit R, Eser S, Mathers C, et al. GLOBOCAN 2012 v1.1, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 11 [Internet]. Lyon, France: International Agency for Research on Cancer; 2014.
- Institute for Science, Engineering and Public Policy [Internet]. Portland Oregon: ISEPP, 2007. Decoding Life: The Next Phase of Discovery [cited 2016 Oct 15]. Available from: https://www.isepp.org/Pages/07-08%20Pages/Venter.html.
- Hamilton AS, Mack TM. Puberty and genetic susceptibility to breast cancer in a case-control study in twins. N. Engl. J. Med. 2003 Jun 5;348(23):2313-22.
- Willett WC. Diet and cancer. Oncologist. 2000;5(5):393-404.
- Curado MP, Edwards B, Shin HR, Storm H, Ferlay J, Heanue M, et al. IARC Scientific Publications No. 160. Vol. IX. Lyon: IARC; 2007. Cancer incidence in five continents.
- Divisi D, Di Tommaso S, Salvemini S, Garramone M, Crisci R. Diet and cancer. Acta Biomed. 2006 Aug;77(2):118-23.
- Belpomme D, Irigaray P, Hardell L, Clapp R, Montagnier L, Epstein S, Sasco AJ. The multitude and diversity of environmental carcinogens. Environ. Res. 2007 Nov;105(3):414-29. Epub 2007 Aug 9.
- Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003 Apr 24;348(17):1625-38.
- Booth W, Chakravarthy MV, Gordon SE, Spangenburg EE. Waging war on physical inactivity: using modern molecular ammunition against an ancient enemy. J. Appl. Physiol. 2002 Jul;93(1):3-30.
- Van der Pols JC, Bain C, Gunnell D, Smith GD, Frobisher C, Martin RM. Childhood dairy intake and adult cancer risk: 65-y follow-up of the Boyd Orr cohort. Am J Clin Nutr. 2007 Dec. 86(6):1722-9.
- Colditz GA, Cannuscio CC, Frazier AL. Physical activity and reduced risk of colon cancer: implications for prevention. Cancer Causes Control. 1997 Jul;8(4):649-67.
- Harikumar KB, Aggarwal BB. Resveratrol: A multitargeted agent for age-associated chronic diseases. Cell Cycle. 2008 Apr 15;7(8):1020-35. Epub 2008 Feb 15.
- McIntyre A, Gibson PR, Young GP. Butyrate production from dietary fibre and protection against large bowel cancer in a rat model. Gut. 1993 Mar; 34(3): 386–391.
- Miller HE, Rigelhof F, Marquart L, Prakash A, Kanter M. Antioxidant content of whole grain breakfast cereals, fruits and vegetables. J. Am. Coll. Nutr. 2000 Jun;19(3 Suppl):312S-319S.
- Slavin JL, Jacobs D, Marquart L, Wiemer K. The role of whole grains in disease prevention. J. Am. Diet Assoc. 2001 Jul;101(7):780-5.
- Willett W. The search for the causes of breast and colon cancer. Nature 1989 Mar 30;338(6214):389-94.
- Bostick RM, Potter JD, McKenzie DR et al. Reduced risk of colon cancer with high intake of vitamin E—the Iowa Womens’ Health Study. Cancer Res.1993 Sep 15;53(18):4230-7.
- Ip C. The chemopreventive role of selenium in carcinogenesis. J Am Coll Toxicol. 1986; 206:431-47.
- Clark LC. The epidemiology of selenium and cancer. Fed Proc. 1985 Jun; 44(9):2584-9.
- Hyman J, Baron JA, Dain BJ et al. Dietary and supplemental calcium and the recurrence of colorectal adenomas. Cancer Epidemiol. 1998 Apr 7;(4):291-5.
- Bostick RM. Effects of Supplemental Vitamin D and Calcium on Normal Colon Tissue and Circulating Biomarkers of Risk for Colorectal Neoplasms. The Journal of steroid biochemistry and molecular biology. 2015;148:86-95. doi:10.1016/j.jsbmb.2015.01.010.
- Giovannucci E, Stampfer MJ, Colditz GA et al. Multivitamin use, folate, and colon cancer in women in the Nurses’ Health Study. Ann Intern Med. 1998 Oct 1;129(7):517-24.
- Valle L. Genetic predisposition to colorectal cancer: Where we stand and future perspectives. World Journal of Gastroenterology : WJG. 2014;20(29):9828-9849.
- Cancer Reasearch UK [Internet]. High risk groups for bowel cancer [cited 2016 Nov 15]. Available from https://www.cancerresearchuk.org/about-cancer/type/bowel-cancer/about/risks/high-risk-groups-for-bowel-cancer#cbWXBjDUMv7hAFzQ.99
- Hong, T, Clark, J, Haigis K. Cancers of the Colon and Rectum: Identical or Fraternal Twins?. Cancer Discovery. 2012. 2(2):117-21

Comments