Diet and Lifestyle Can Prevent Breast Cancer
Breast cancer doesn't occur overnight. Many years can pass before a palpable lump forms. But lifestyle changes can prevent it from developing further.

Table of contents
Conclusions
Many years can pass between the time the first cell starts to multiply erratically and a palpable lump forms. In this period, lifestyle changes and a healthy diet can prevent breast cancer from developing further.
Various studies have shown that smoking, drinking alcohol, and consuming animal products represent significant risk factors for the development of breast cancer.1 Even if it is still a controversial issue, multiple research studies have confirmed the negative impact of milk and dairy products on the development of breast cancer.
A vegan diet is proven to significantly reduce this risk. Scientists recommend cruciferous vegetables as these not only prevent breast cancer but also combat existing tumors.2 It has also been shown that the consumption of flaxseed, dietary fiber 3 and berries has a positive effect in the prevention of breast cancer.
| Not only vegans and vegetarians should read this: A Vegan Diet Can Be Unhealthy. Nutrition Mistakes. |
How breast cancer develops
Each year, around 230'000 women in the United States are diagnosed with breast cancer. And 40'000 of them die from breast cancer.4 Like many other tumors, breast cancer starts with a single cell that divides. With each division, a tumor can double in size.5 This process can take between days and years.
Cancer develops in three phases:
- Initiation: genotoxic carcinogens modify the DNA. A mutation takes place.
- Promotion: the promoters (e.g., "growthhormones") stimulate the growing of the initial cells. Read more here about the "growthhormones" in milk and the way dairy products are detrimental to our health.
- Progression: the invasive tumor spreads into the surrounding tissue (metastasis) or forms distant metastases.5
The mammary glands change constantly, from life in the uterus until menopause. Under the influence of diet and lifestyle and during any of the phases in a personʼs lifespan, but primarily during fetal development, puberty, and pregnancy, an epigenetic modification can take place. This can then lead to a higher risk of developing cancer.
What is epigenetic modification?
Epigenetics studies genetic effects not encoded in the DNA sequence of an organism, hence the prefix epi- (Greek: επί- over, outside of, around). Such effects on cellular and physiological phenotypic traits may result from external or environmental factors that switch genes on and off and affect how cells express genes. These alterations may or may not be heritable, although the use of the term epigenetic to describe processes that are heritable is controversial.
6
The term also refers to the changes themselves: functionally relevant changes to the genome that do not involve a change in the nucleotide sequence. Examples of mechanisms that produce such changes are DNA methylation and histone modification, each of which alters how genes are expressed without altering the underlying DNA sequence. Gene expression can be controlled through the action of repressor proteins that attach to silencer regions of the DNA. These epigenetic changes may last through cell divisions for the duration of the cell's life, and may also last for multiple generations even though they do not involve changes in the underlying DNA sequence of the organism; instead, non-genetic factors cause the organism's genes to behave (or "express themselves") differently.
This is why diet and the foods we eat can have an ongoing effect on the risk of breast cancer for many years thereafter, and even for the next generation(s).7
Factors that increase the risk of breast cancer
“The Harvard Report on Cancer Prevention” investigated the impact of various factors on cancer development and was able to determine the main risk areas. The report lists diet and lifestyle (e.g., eating habits, smoking, lack of exercise, alcohol consumption, and a diet rich in salt and food additives) as the strongest factors (69 % *) influencing the process of cancer development.
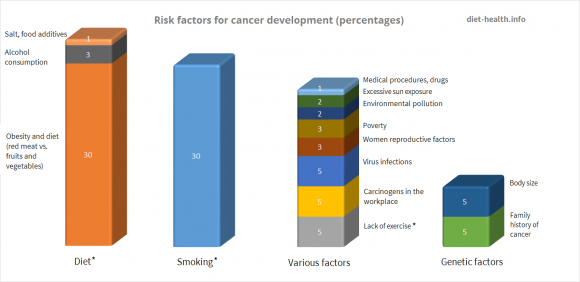
As might be expected, when taken individually, the initiation and development of each type of cancer are determined by a particular cumulus of causes and risk factors, each having different significance levels.
With regard to breast cancer, some of the risk factors include dietary choices (consumption of meat, saturated fats, and dairy versus a vegan diet), alcohol consumption, and body weight.
- A research study conducted in 2002 on a group of 292 British women ages 20–70, showed that “a plant-based (vegan) diet is associated with a lower circulating level of "Insulinlike GrowthFactor" I (IGF-I) compared with a meat-eating or lacto-ovo-vegetarian diet.”8
- Another study9 concluded that a low-fat vegan diet may be especially helpful in protecting against breast cancer because of its capacity to regulate peptid hormone "I" production and high phytochemical content.
- The study, which was conducted over 6.7 years on 30'797 postmenopausal women, ages 50–76 years10, examined the association between AICR’s (American Institute for Cancer Research) recommendations for preventing the most common cancers worldwide and invasive breast cancer incidence. The risk of breast cancer was reduced by 60 % in women who met at least five recommendations related to body fat, plant-based diet, and alcohol, as compared with those who met none of the recommendations.
Taking into consideration the fact that many breast cancers are genetically and epigenetically determined, it is essential to have a diet that not only prevents the initiation, but more importantly, also inhibits the promotion phase (cancerous cell erratic multiplication).
Alcohol consumption, one of the main risk factors for breast cancer
In 2010, the World Health Organization established that the use of alcohol presents a definite risk for cancer 12, and researchers demonstrated this in more than a hundred studies. Even if most of the conclusions were based on studying the effects of moderate and high alcohol intake, it has recently been shown that even light alcohol drinking (defined as up to 1 drink/day) also has the potential to increase the risk of breast cancer.
This can be explained by the process of alcohol metabolism. During the alcohol breakdown process, a highly toxic substance called acetaldehyde forms that is considered to be a promoter for many types of cancer.
The formation of acetaldehyde in the process of alcohol metabolism
Alcohol is metabolized by several processes or pathways. The most common of these pathways involves two enzymes—alcohol dehydrogenase (ADH) and aldehyde dehydrogenase (ALDH). These enzymes help break apart the alcohol molecule, making it possible to eliminate it from the body. First, ADH metabolizes alcohol to acetaldehyde, a highly toxic substance and known carcinogen. Then, in a second step, acetaldehyde is further metabolized down to another, less active byproduct called acetate, which then is broken down into water and carbon dioxide for easy elimination.
(National Institute on Alcohol Abuse and Alcoholism, 2007)
Problems can occur during any of these phases (e.g., inefficient metabolization of substances, elimination problems, or too high a quantity of alcohol that cannot be metabolized efficiently) and cause an excess of acetaldehyde and higher levels of toxicity.
Furthermore, alcohol increases the levels of estrogen and other hormones associated with certain types of breast cancer.
Starting with just three alcoholic beverages per week, the chances of developing breast cancer increase, and for women already diagnosed with early stages of breast cancer the recurrence incidence is higher.
Heating process promotes breast cancer
Heterocyclic amines (HCAs) are chemicals formed when meat (e.g., fish, beef, pork, and poultry) undergoes high temperature cooking processes (e.g., grilling, roasting, or frying). The longer meat is heated at high temperatures, the more HCAs are formed.
PhIP (2-Amino-1-methyl-6-phenylimidazo(4,5-b)pyridine) is one of the HCAs that appear most frequently in meat processed at high temperatures. Similar to estrogen, it attaches to special receptors of breast cancer cells and stimulates their growing.
These findings are supported by two main studies:
- The Long Island Breast Cancer Study Project (2007) showed that women who eat grilled, barbecued, or smoked meats during their lifetime may have a 47 % higher risk of breast cancer.13
-
The Iowa Women’s Health Study determined that women who preferred their meat “well done” (over 90 °C) have a five times higher chance of developing breast cancer than women who prefer their meat rare or medium (52–54 °C).14
Excess weight leads to an increased risk of breast cancer in postmenopausal women
If a person is overweight, eating a healthy diet might not reduce their risk of breast cancer. A study conducted in 2004 on approximately 9'000 women17 showed that when the BMI is lower than 25 kg/m2, a healthy diet can lower the risk of breast cancer; however, there is no significant impact when the BMI is over 25 kg/m2.
Epidemiological studies have also provided evidence that obesity during pregnancy influences obesity in children, which may have consequences for the risk of breast cancer in the next generation.7
High intake of refined carbohydrates is associated with risk of breast cancer
A high intake of refined carbohydrates leads to high "insulinlevels". Chronically high "insulinlevels" may increase the formation of cancerous cells in the breast and promote the availability of IGF-1 ("InsulinlikeGrowthFactor" 1), which stimulates cell growing and proliferation. 16
Processed meat, fish, butter, animal fats, and margarine — double the risk of breast cancer
The European Prospective Investigation into Cancer and Nutrition (EPIC) Study, which registered and analyzed the dietary patterns of 15'352 female subjects over a period of six years, showed that eating habits characterized by high consumption of processed meat, fish, butter, animal fats, and margarine are responsible for more than 42 % of the total fat intake. This was associated with an increased risk of breast cancer.18
Milk consumption as a possible risk for breast cancer
There are multiple studies directly linking milk consumption to the development of breast cancer, but there is still much controversy and need for further scientifically grounded research.
The main reasons why milk might have such a strong impact on the development of cancer are as follows:
- Milk and dairy products contain high levels of estrogen metabolites, which are absorbed by the human body and lead to hormonal imbalances. Furthermore, estrogen stimulates the growing of breast cells, and as a result also the growing of hormone-receptor-positive breast cancer cells.
Modern genetically improved dairy cows continue to lactate throughout almost the entire pregnancy. Therefore, recent commercial cow's milk contains large amounts of estrogens and progesterone
19. Read more here about how the genetically “improved” cattle and industrialized milk production has significantly changed the impact of milk on human health. - Whole milk and dairy products (e.g., cheese, butter, and quark) contain a relatively high proportion of unsaturated fatty acids which, together with those found in meat, were positively correlated with an elevated risk of breast cancer.21
- Milk and dairy products are prone to be contaminated with persistent residues and pesticides, which bear an influence on breast cancer incidence.
- Milk also contains "Insulinlike GrowthFactor" 1 (IGF-1), which has "growthpromoting" properties. It is known that women with high levels of IGF-1 in their blood may have a higher risk of breast cancer 20, and it is also thought that high IGF-1 levels might cause existing cases of breast cancer to spread.
How nutrition helps prevent breast cancer
Based on the above risk factors, researchers from the American Institute for Cancer Research (AICR)1 established a list with recommendations regarding breast cancer prevention. The four most important are eating a vegan diet, not smoking (or chewing tobacco), getting regular physical activity, and not drinking alcohol.

Cruciferous vegetables fight tumors
Researchers have found that cruciferous vegetables such as broccoli and brussels sprouts not only help prevent the development of breast cancer, but can also help fight existing tumors. Cruciferous vegetables contain large quantities of sulforaphane, a substance that activates the body’s detoxification enzymes in the liver. These help neutralize the heterocyclic amines (HCAs).
A study involving nonvegan subjects showed that the level of HCAs in urine is lower when people consume three cups of broccoli or brussels sprouts daily in addition to their regular meat-based meal.2
Soy intake — a controversial impact on breast cancer
Most studies suggest that a higher intake of soy isoflavone is associated with a lower risk of breast cancer. However, other research shows that this applies only to the Asian population, and that among Western women an increase of soy consumption has no impact on cancer risk. 22
Given the potential for estrogenic activity, there is special concern that soy consumption might increase the risk of breast cancer in postmenopausal women. Nevertheless, clinical trials developed over periods between one and three years have shown soy to have no impact on breast density.
Dietary fiber reduces the risk of breast cancer
The consumption of dietary fiber has a significant impact on estrogen receptor-negative breast cancer.
In one study, researchers from Yale University showed that premenopausal women who consume more than 6 grams of fiber per day (the equivalent of a cup of black beans) have a 62 % lower risk of breast cancer than women who consume just 4 grams of fiber.
A diet high in lignans could prevent breast cancer and reduce its evolution
Lignans are phytonutrients (phytoestrogens) with a structure and impact similar to that of estrogen. As a result, they can attach to the estrogen receptors in cells. But unlike the more aggressive estrogen, the lignans have a weaker effect.
And since the receptors are already occupied by the lignans, the aggressive estrogen that leads to breast cancer cannot exercise its carcinogenic effects and ends up being broken down by the body.
The foods with the highest lignan content are flaxseed, berries, grains, nuts, and broccoli.
In this study, 45 women with a high risk of developing breast cancer were tested. They were required to consume two teaspoons of flaxseed per day. Biopsies of the breast tissue were performed at the beginning of the study and after one year.
At the end of the study, 80 % of the subjects had a lower risk of developing cancer, based on the lower levels of Ki-67, an indicator of cell proliferation.
Thanks to the high amount of lignans it contains, Erb Muesli is a perfect breakfast and a healthy way to start the transition to a diet that has the capacity to prevent or reverse breast cancer.
Vitamin D is associated with a reduced risk of breast cancer
Both, vitamin D synthesized from sun exposure and dietary vitamin D are converted in the liver to 25-hydroxyvitamin D (25OHD).
However, the Nurses’ Health Study, which examined 90'000 subjects and had a 14-year follow-up, showed that a higher intake of vitamin D only has a relevant impact on premenopausal women, while the impact is irrelevant in postmenopausal women.
Nutrient-dense foods have fewer calories. High-calorie foods have fewer nutrients.
A plant-based diet provides valuable fiber as well as vitamins and minerals. In contrast, animal products such as meat, fish, and eggs provide virtually no fiber. And even though the calorie intake is often higher when a person consumes animal products, their body can easily become depleted of many vital nutrients found in plants, nuts, seeds, and legumes.
In addition, a whole foods and plant-based diet tends to promote a healthy body mass index, which is associated with a lower risk of breast cancer.
Read more here about how raw food could beneficially impact your health.
Daily dietary recommendations for preventing breast cancer
Based on comprehensive research of breast cancer survivors, Bodai and Tuso24 have made daily dietary recommendations to help improve overall health, prevent cancer development, and increase long-term survival rates of individuals who have already been diagnosed with cancer:
| Decrease or eliminate | Increase |
| Unhealthy carbohydrates | Healthy carbohydrates |
|
|
| Unhealthy fats | Healthy fats |
|
|
| Salt, meat, dairy, and alcohol |
Special attention should be paid when making generalizations about the impact of diet on breast cancer. The results of many studies are in direct correlation with a specific type of breast cancer, apply to specific populations of women, and are dependent on the life stage of the patient (e.g., premenopausal or postmenopausal).
Other factors such as the amount of a special nutrient, timing, association with other nutrients, life history, and diet in the early stages of life could significantly alter the impact of diet on breast cancer.
Literature — sources:
24 sources
- American Institute for Cancer Research [Internet]. Recommendations for Cancer Prevention; 2014, September 12 [cited 2016, July 20]. www.aicr.org/ can-prevent/ what-you-can-do/10-recommendations.html.
- Murray S, Lake BG, Gray S, Edwards AJ, Springall J, Bowey EA, et al. Effect of cruciferous vegetable consumption on heterocyclic aromatic amine metabolism in man. Carcinogenesis. 2001 Sep; 22(9): 1413-20.
- Thompson LU, Chen JM, Li T, Strasser-Weippl K, Goss PE. Dietary flaxseed alters tumor biological markers in postmenopausal breast cancer. Clin Cancer Res. 2005; 11(10): 3828-35.
- American Cancer Society [Internet]. Breast Cancer Facts & Figures 2013-2014. [cited 2016 July 19]. www.cancer.org /acs/groups/content /@research/documents /document/ acspc-042725.pdf.
- Friberg S, Mattson S. On the "growthrates" of human malignant tumors: implications for medical decision making. J Surg Oncol. 1997; 65(4): 384-97.
- Wikipedia [Internet]. Epigenetics. [cited 2016 October 31]. Available from: https://en.wikipedia.org /wiki/Epigenetics
- Teegarden D, Romieu I, Lelièvre SA. Redefining the impact of nutrition on breast cancer incidence: is epigenetics involved? Nutrition research reviews. 2012;25(1):68-95.
- Allen NE, Appleby PN, Davey GK, Kaaks R, Rinaldi S, Key TJ. The associations of diet with serum "InsulinlikeGrowthFactor I" and its main binding proteins in 292 women meat-eaters, vegetarians, and vegans. Cancer Epideminol Biomarkers Prev. 2002; 11(11): 1441-8.
- McCarty MF, Vegan proteins may reduce risk of cancer, obesity, and cardiovascular disease by promoting increased glucagon activity. Med Hypotheses. 1999 Dec; 53(6):459-85.
- Hastert TA1, Beresford SA, Patterson RE, Kristal AR, White E. Adherence to WCRF/AICR cancer prevention recommendations and risk of postmenopausal breast cancer. Cancer Epidemiol Biomarkers Prev. 2013 Sep;22(9):1498-508.
- Havard Center for Cancer Prevention. Harvard Report on Cancer Prevention, Causes of human cancer. Cancer Causes & Control. 1996; 7(1): 3-59.
- International Agency for Research on Cancer. Lyon, France. 2010. Alcohol Consumption and Ethyl Carbamate. Monographs on the Evaluation of Carcinogenic Risks to Humans, Vol 96.
- Bagnardi V, Rota M, Botteri E, Tramacere I, Islami F, Fedirko V, et al. Light alcohol drinking and cancer: meta-analysis. Ann Oncol. 2013; 24(2): 301-8.
- Zheng W, Gustafson DR, Sinha R, Cerhan JR, Moore D, Hong CP, et al. Well-done meat intake and the risk of breast cancer. J Natl Cancer Inst. 1998; 90(22): 1724-9.
- Trentham-Dietz A, Newcomb PA, Egan KM, Titus-Ernstoff L, Baron JA, Storer BE, et all. Weight change and risk of postmenopausal breast cancer (United States). Cancer Causes Control. 2000 Jul; 11(6):533-42.
- Gallagher EJ, LeRoith D. The Proliferating Role of I- and "InsulinLike GrowthFactors" in Cancer. Trends in endocrinology and metabolism: TEM. 2010;21(10):610-618.
- Sieri S, Krogh V, Pala V, Muti P, Micheli A, Evangelista A, et al. Dietary patterns and risk of breast cancer in the ORDET cohort. Cancer Epidemiol Biomarkers Prev. 2004;13:567–572.
- Schulz M, Hoffmann K, Weikert C, Nöthlings U, Schulze MB, Boeing H. Identification of a dietary pattern characterized by high-fat food choices associated with increased risk of breast cancer: the European Prospective Investigation into Cancer and Nutrition (EPIC)-Potsdam Study. British Journal of Nutrition. 2008; 100(5): 942–946.
- Maruyama K, Oshima T, Ohyama K: Exposure to exogenous estrogen through intake of commercial milk produced from pregnant cows. Pediatr Int 2010; 52:33–8.
- Boyd NF, Stone J, Vogt KN, Connelly BS, Martin LJ, Minkin S. Dietary fat and breast cancer risk revisited: a meta-analysis of the published literature. Br J Cancer. 2003;89:1672–85.
- Yu H, Rohan T. Role of the "InsulinLike GrowthFactor" Family in Cancer Development and Progression. JNCI J Natl Cancer Inst. 2000; 92(18): 1472-1489. doi: 10.1093/jnci /92.18.1472
- Dong JY, Qin LQ. Soy isoflavones consumption and risk of breast cancer incidence or recurrence: a meta-analysis of prospective studies. Breast Cancer Res Treat. 2011;125:315–323.
- Garland CF, Gorham ED, Mohr SB, Grant WB, Giovannucci EL, Lipkin M, et all. Vitamin D and prevention of breast cancer: pooled analysis. J Steroid Biochem Mol Biol. 2007 Mar; 103(3-5):708-11.
- Bodai BI, Tuso P. Breast Cancer Survivorship: A Comprehensive Review of Long-Term Medical Issues and Lifestyle Recommendations. The Permanente Journal. 2015;19(2):48-79. doi:10.7812/TPP/14-241.

Comments