Book review of “Milk, Money, and Madness” by N. Baumslag
With overwhelming evidence, Dr. Baumslag explains how important breast-feeding is and why baby formula is problematic—something an expecting mother should know!

Table of contents
- Conclusion
- 1. Summary
- 2. Book review
- Section 1: Breastfeeding Beliefs and Practices
- 2.1. Breastfeeding Beliefs and Practices
- 2.2. Wet Nursing, Surrogate Feeding, and Healing Qualities of Breastmilk
- Section 2: Breastmilk: The Miracle Food and Medicine
- 2.3. “Cow's Milk Is for Cows”
- 2.4. Artificial Feeding
- Section 3: Breastmilk Economics — Shaping Corporate and Governmental Policies
- 2.5. The Global Search for Formula Sales
- 2.6. Women and Work
- 3. About the book
Conclusion
Based on scientific studies, this book documents the importance of breast-feeding infants for a longer period of time than is customary in our society. It would be optimal for infants to be breast-fed for one year; however, they can be given supplementary food after a few months.
This book doesn’t deal with the transition period that a woman who has just given birth goes through (postnatal period, postpartum period), but instead describes the importance of colostrum and of breast milk, which is specially designed for the child.
We also learn much practical information about breast-feeding.
If you want to learn about the health problems that milk and dairy products can cause in children and adults, you should read the book "Milch besser nicht!" (Milk, better not) by Maria Rollinger — or at least this book review of her book.

1. Summary
The authors draw from 190 books and articles, which they list by chapter in the reference section at the end of the book. Professor Naomi Baumslag is a pediatrician who, along with her position as a university professor, works in international organizations such as USAID, UNICEF, and WHO. For many years, she has been the president of WPHN, the very successful Women’s International Public Health Network. She has also gained extensive practical experience in numerous countries around the globe.
The book examines practically all aspects and practices related to breast-feeding (nursing) and bottle-feeding (baby formula, infant formula, and “follow-up” milk) babies and toddlers.
It shows the reasons behind the very different traditions when it comes to the female breast, breast-feeding, and infant nutrition. A related topic is sexual behavior during both pregnancy and breast-feeding in different cultural areas, ethnic groups, and times (philosophy of space and time and arrow of time).
It is interesting that social behaviors usually don’t reflect our natural needs. Depending on the zeitgeist (spirit of the time) and religion, there are a number of very different customs. However, unnatural practices are often linked to a higher and unnecessary infant mortality rate. The book describes poor options for infant nutrition and the serious consequences of such. We also learn how important it is to have flexible breast-feeding times.
The book also covers reasons why it is important to breast-feed for a longer period of time and for the baby to be close to the mother (cosleeping). This helps to synchronize the sleep patterns (wakefulness, sleep, and sleep stages) of the mother and child. The child doesn’t have any reason to cry, and the mother and child can sleep longer in the morning without disturbing the rest of the family.
The text also describes the different ways to stimulate milk flow. These and other aspects are difficult for the Western world to understand at the current time.
Various practices such as having wet nurses lead us far back in history and introduce us to customs other than our own. We read about practices still carried out today as part of breast-feeding that we would never have believed existed.
The book and this text show readers why formula milk has experienced and continues to experience such great popularity, even though it does not offer the same quality and can never completely replace breast milk. There are very logical reasons supported by scientific evidence for the superiority of breast milk.
We also read the story of the boycotts against manufacturers with information about how infants who receive formula have much higher sickness and death rates.
And finally we learn why paid maternity is so important and that up until at least the middle of the 1990s the majority of women did not receive this in the United States.
About the authors
Naomi Baumslag, M.D., M.P.H., is a Clinical Professor of pediatrics at Georgetown University Medical School in Washington, DC. She is president of the Women’s International Public Health Network (WIPHN) (for 2015 as well) in Bethesda, Maryland.
She has also served in an advisory capacity for the USAID, UNICEF, and WHO, the Georgia Department of Human Resources, the PAHO Foundation (prev. PAHEF), and for government agencies in many developing countries, as well as on the Health Council of La Leche League International (LLLI) and the World Alliance for Breastfeeding Action (WABA).
Professor BAUMSLAG has written more than 100 articles und eight books. She also gives lectures, both internationally and in the United States.
DIA L. MICHELS is a science writer for newspapers and magazines around the world. Her commitment to breast-feeding stems both from her own research and her personal experience of breast-feeding her own children over the past six years.
This is the second book she has coauthored with Professor BAUMSLAG. In 1992, the authors published "A Woman’s Guide to Yeast Infections", Pocket Books (288 pages).

According to Open Library, the author Dr. Naomi Baumslag also wrote the following books:
- Murderous Medicine (2005),
- Primary Health Care Pioneer (1986),
- A Woman’s Guide to Yeast Infections (1992),
- Family Care (1973).
2. Book review
It is generally thought that breast-feeding is an instinctual process that is driven by hormones. However, the authors explain how breast-feeding is actually something that has to be learned. Other primates also have to learn how to breast-feed. Changing views on the subject also play a role. The female breast has been transformed into a sex symbol in many time periods (zeitgeist) and societies.
Section 1: Breastfeeding Beliefs and Practices
Section 1 is divided as follows:
Part 1 (here 2.1):
Breastfeeding Customs around the World; Breasts as Sex Symbols; Intercourse Taboos; Diet during and after Pregnancy; Cravings in Pregnancy; The Fear of Labor and Delivery; Childbirth Assistance; Mothering the Mother; Galactagogues (substances that promote lactation); Beliefs about Colostrum (first milk); Premature and Small Infants (preterm birth and neonatology); Is the Milk Good Enough? (breast milk); Feeding Styles; Carrying Baby; Swaddling; and Duration of Breastfeeding
Part 2 (here 2.2):
Wet Nursing, Surrogate Feeding, and Healing Qualities of Breastmilk; Selection of Wet Nurses; Slaves as Breeders and Feeders; Do You Have to Have a Baby to Breastfeed?; Surrogate Feeding; Breastmilk Pumps; Breastmilk Banks; Interspecies Nursing; Nursing the Aged; and The Healing Qualities of Breastmilk
2.1. Breastfeeding Beliefs and Practices
The authors show the strong influence that religion and customs have on birth and motherhood. For example, Jews who live in accordance with the Talmud (Torah) are supposed to breast-feed their children at least two years (p. 5). In many societies around the globe, it is the well-off and affluent families, in particular, who have a distaste for breast-feeding.

Although we know that children who are breast-fed for a longer period have a better life expectancy, breast-feeding and the length of such change based on current trends. At times, breast-feeding has been seen as disgusting, unwomanly, or unhealthy
(p. 5).
For instance, many rich Chinese women were not able to breast-feed their children at all because they wore very tight dresses that completely flattened their breasts.
The breast has been transformed into a sexual object
In the United States, women, at least in certain states, have not been allowed to breast-feed in public.
For example, one woman who was nursing her child in her own parked car was warned by a police officer that she was in danger of breaking indecent exposure laws. The breast has been transformed into a sexual object.
In the early 1980s, the Food and Drug Administration (FDA) received the following message from the American Society of Plastic Surgeons (ASPS):
There is a substantial and enlarging body of medical information and opinion to the effect that these deformities [small breasts] are really a disease [that left uncorrected, results in a] total lack of well being (p. 7)
In other words, small breasts are a disease that needs to be cured.
This organization has had much success. In 1990 alone, a total of 130'000 women in the United States had operations to have their breasts enlarged. The FDA did not even begin to intervene in spite of the negative health consequences and reports of fatalities.
The authors discuss the issue of intercourse taboos during breast-feeding. There are indeed good reasons for restricting coital relations since children who are born too soon after their next older sibling have a significantly higher death rate in developing countries and are often later neglected.
The same thing happens when children aren’t breast-fed or are breast-fed for too short of a time. The book provides some related statistics and specific examples from various cultures.
Intercourse taboos
In several tribes in Africa, in particular, there is an intercourse taboo during the breast-feeding period. For example, in the Zulu tradition, it is believed that a man will become impotent if a drop of breast milk falls on his skin (p. 8).
Men have pressured their nursing wives for decades to accelerate the weaning process by switching over to formula, which is good for our dairy companies.
In addition, women on birth control pills that contain estrogen (oestrogen) produce a significantly lower amount of milk.
And in many cases, women who give birth (delivery) in hospitals are seen as “cleaned out” and the traditional intercourse taboos no longer apply (p. 10). This means that the time until the next child is born will most likely be shorter — with all of the disadvantages this brings.
The hormone "oxytoc..", which is produced for the birthing process and during breast-feeding, helps nursing mothers to feel calm and nurturing. However, it also reduces vaginal lubrication, which can make sex uncomfortable. Nature has actually provided a process that allows a child to better develop, without a second pregnancy occurring too soon. But we ignore this natural process (p. 10).
The diet restrictions for pregnant and nursing mothers vary widely in different regions and time periods. In certain areas in Tunisia, women don’t eat eggs, whereas in another region, the opposite is true and nursing women are encouraged to eat between six and eight eggs daily.
The authors discuss entirely absurd and harmful customs as well as beneficial practices.
Alcohol, cow milk and coconuts
We haven’t known for so long that when pregnant mothers drink alcohol, it can cause problems for the child — to a smaller extent, this can also happen when nursing mothers drink alcohol.
In Sierra Leone, pregnant women aren’t allowed to drink alcohol.
In Sri Lanka, nursing mothers are prohibited from drinking cow milk, and in other regions coconuts are off limits. Both of these foods can cause allergic reactions (p. 13).
In the next subsection, the authors deal with the special food cravings that pregnant women have. Many of these are still unexplained, but others are backed up by science.
In as early as about 400 CE, Plato wrote that he had seen pregnant women eating dirt. This craving for “dirt” can be explained by the fact that dirt contains vitamin B12 and other minerals that may be lacking in some women’s diets.
The practice of eating clay
The practice of eating clay is also well known and was popular among African American women.
Clay contains a high amount of iron and also chemical elements (trace elements) such as sodium (Na), manganese (Mn), arsenic (As), silver (Ag), molybdenum (Mo), and uranium (U).
Because of its high pH, clay also has an antibacterial effect. Recent studies have indeed shown that clays rich in iron from several deposits have this effect.

Sodium is one of the elements that is essential for all animal organisms.
Manganese is an essential element for all living things and a component of various enzymes.
Arsenic is a trace element in humans, but its biological significance for us has not yet been fully established.
Arsenic is also an essential element for many animals.
Silver is used as the color additive E 174 in the food industry, for example, for the shells of sweets such as pralines and in licorice.
Molybdenum is a trace element that is essential for almost all living organisms as it is a component of the active site of a number of enzymes such as nitrogenase, nitrate reductase, and sulfite oxidase.
In the Brothers Grimm fairy tale Rapunzel, the expecting mother looks pale and weak. The father to be steals rampion leaves (campanula rapunculus) from the neighbor’s garden.
Today we know that rampion leaves and other green vegetables are rich in folic acid (vitamin B9 or folate).
Campanula rapunculus
 | Wikipedia (English entry): Campanula rapunculus, common name rampion bellflower, rampion, or rover bellflower, is a species of bellflower (Campanula) in the family Campanulaceae. |
The authors look briefly at the methods of the German physician Prochownik who restricted the caloric intake of pregnant women who had a small or contracted pelvis. His of goal was to reduce the weight of newborns so that mothers would have an easier birth. This was in some cases tragic for the children. Pelvic distortion can result from rickets, a disease caused by lack of sunlight and/or Vitamin D, calcium, or potassium.
(p. 14).
Childbirth assistance and support provided to young mothers by relatives are also topics that are very much in contrast to today’s industrialized society.
Colostrum, the milk produced during the first few days, is increasingly being recognized as important for an infant’s health. It was long believed that this milk, which has a different color and flows somewhat thicker, was harmful for the child. This is why colostrum has been withheld in certain times and cultures. However, the practice leads to many early deaths and children who later have a weaker immune system.
Similar serious mistakes made in other cultures
The Indian system of Ayurvedic medicine (Ayurveda) also believed colostrum to be harmful: As far back as the second century BC, Indian Ayurvedic medicine recommended honey and clarified butter for the newborn's first four days, during which the birth mother's colostrum was expressed and discarded
(p. 24).
This also happened in biblical times. The authors describe similar serious mistakes made in other cultures, for example, in Guatemala, Afghanistan, Sierra Leone, and Lesotho.
And Greek, Roman, and later French, English, and other European physicians recommended the same course of action up until the eighteenth century — without stopping to question the practice.
The British physician Dr. Ettmueller came into serious conflict with the medical establishment of the time when in 1699 he recommended that newborns should be breast-fed and receive colostrum from the beginning.
Another 50 years would have to pass until a similar call to action by the physician William Cadogan in 1748 would turn out to be more effective:
The mother’s first milk is purgative and cleanses the child of its long hoarded excrement; no child can be deprived of it without manifest injury (p. 24).

Wikipedia cites William Cadogan (1711–1797) as the first physician who advocated the complete abolition of swaddling. He did so in an essay in 1748 titled "An Essay upon Nursing and the Management of Children, from their Birth to Three Years of Age".
Before this time, people were obliged to strictly follow this practice.
Early childhood mortality had previously been very high; Fildes showed in 1980 that just this one step reduced childhood mortality (infant mortality) by 16 %.
But mothers also take part in other practices, with the support of the industry, that are not in the best interest of the child. An example of this is the sugar water bottles that infants in the United States receive when they are still in the hospital. These make it easier to care for the babies as they are quieter – but it is to their detriment. It gets them used to taking a bottle instead of breast-feeding ...
In seldom cases, this can bridge the time until the breast milk comes in. But new babies usually don’t need any fluids besides breast milk, even in hot climates. And this breast milk should come from the baby’s own mother if possible, even if the milk doesn’t come in immediately.
The authors then turn to the topic of premature and small infants (p. 25). In particular, they criticize the fact that pediatricians only look at weight gain and, if they are not satisfied with this, they recommend supplementing with formula rather than examining the mother’s health and eating habits and suggesting changes as necessary. Ironically, this was recommended by Soranus von Ephesos eighteen centuries ago.
Demand feeding
At the beginning of the twentieth century, the physician Truby King from New Zealand popularized the harmful practice of nursing babies every four hours and encouraged mothers to stop the practice of demand feeding.
In addition, nurses analyzed the fat content of the milk and prescribed supplementary feeding.
Again this was done instead of giving the mothers nutrition advice and finding out more about their environment. These were also standard practices in England (pp. 28 and 128).
The authors give an overview of other changes and differences related to breast-feeding and carrying infants that are found in diverse cultures. They regret that infants no longer sleep in a family bed as was traditional. Disruptions caused by breast-feeding are much smaller when the baby is in the parent’s bed because the baby receives milk as soon as it needs it and doesn’t have to be moved.
Studies suggest that mothers and their babies have a mysterious connection that is caused by prolactin (PRL) and seem to dream in unison and both know when milk is needed. The sleeping cycles of the mother and child are similar so that they can both get the periods of deep sleep (hypnogram and polysomnography, PSG), which are needed for overall health (p. 31).
Our inner clock and the symbiosis between mother and child
Our inner clock ensures that we maintain a stable 24-hour rhythm, for example, of sleep and wakefulness and is also responsible for many endocrine processes such as the production of cortisol and melatonin.
The functions of our central nervous system show clear, endogenously controlled daily rhythms, which are called circadian clocks (circadian rhythms).
See also circadian rhythm sleep disorder, Neurologie der Bindung (Neurology behind the connection between mother and child, German only), and cosleeping.
I find that sleep training is the wrong method as it isn’t natural, even if nobody has published studies on this topic ...
The central circadian clock is found in the suprachiasmatic nucleus (SCN) of the ventromedial hypothalamus. Nerve cells in the SCN rhythmically express clock genes.
Molecular circadian rhythms are also found in peripheral organs such as the liver, pancreas, kidneys, adrenal glands, heart, and lungs. The hypothalamus controls these peripheral clocks.
A chronic disorder of the circadian rhythms can cause a higher rate of heart and circulation disorders, obesity, type-2 diabetes, and cancer.
The clock gene was first researched in the Drosophila melanogaster.

On the symbiosis between mother and child from Wikipedia (German version): Margaret Mahler sets the beginning of the symbiotic phase at around two months, during the oral phase. At this time, the child is physically and mentally dependent on the mother.
"It cannot yet distinguish between inside and outside, between itself and objects, or between itself and its mother. It experiences the mother as part of its own self, and has an inseparable symbiotic unity with her."
"The mother must be able to recognize the child’s needs in order to ensure that it is satisfied and healthy since the child has not yet developed conscious thinking. If the mother is available to the child during the symbiotic phase, the child can develop basic feelings of security and trust. The relationship between mother and child serves as the foundation for later relationships."
See also Erikson’s stages of psychosocial development from the psychoanalyst Erik H. Erikson (1902–1994).
The authors write that it is fortunate that swaddling is no longer widely practiced, and they describe reasons why it was introduced in many cultures. However, the authors write, Swaddling is not good for children. In addition to hampering normal muscle development and coordination, swaddling can lead to a variety of medical problems involving the lungs, arteries, and veins
(p. 35).
Children must receive breast milk and be free to move
The renowned anthropologist Ruth Fulton Benedict (1887–1948) commented that women have expressed their fundamental values in their swaddling techniques.
As examples, Benedict describes swaddling practices in Russia and Rumania.
In the 1740s, the physician William Cadogan at Foundling Hospital in London warned that children must receive breast milk and be free to move.
Nevertheless, swaddling is still practiced today in some areas of Eastern Europe, in Asia, and in the Middle East in countries such as Mongolia, Afghanistan, Turkey, and Greece.
How long should infants be breast-fed? This is a question that is asked time and time again and that the U.S. Surgeon General Dr. Antonia Novello answered as follows in 1990:
The American Academy of Pediatrics says that babies should be breastfed until age one. … It’s the lucky baby I feel who continues to nurse until he’s two (p. 35).
Customs are very dependent on cultural attitudes. The authors agree with this statement and give reasons why infants should be exclusively breast-fed until they are six months old. At that point, food should be gradually introduced.
A healthy mother with enough milk can also exclusively breast-feed for longer, but after nine months exclusive breast-feeding should be questioned. Continued breast-feeding (along with food) after six months is still always the best method.
Breast-feeding practices
How just very different breast-feeding practices are can be seen in the fact that as late as the 1820s English women in East Lincolnshire apparently let their children drink breast milk until they were seven or eight years old. In the Solomon Islands, breast-feeding was continued until children were 15.
But in 1991, a mother in Syracuse, New York, was found guilty of neglect for breast-feeding her child for more than two years. Her child was even taken from her and placed with a foster care family for a short time.
This can lead to appalling inequality as UNICEF shows with an example from Children’s Hospital Islamabad in Pakistan. The doctor had advised a mother to do so, which led to her daughter suffering from malnutrition (marasmus) and dying. The authors have included a photo on page 37 that the mother gave to UNICEF to use as a warning in their publications.
2.2. Wet Nursing, Surrogate Feeding, and Healing Qualities of Breastmilk
Wet nursing (wet nurse) came into being to save children when their mother had died or wasn’t able to give milk. Later, wealthy families turned this into the standard practice. For example, the pharaohs in Egypt had wet nurses raise their children.
Today, people in the West don’t quite know what to think about surrogate mothers and have mixed feelings on the subject. The reasons for wet nursing were and are to provide an infant with breast milk who would otherwise not receive any and to try to decrease the number of deaths caused by a lack of breast milk.
The topic of wet nurses and practices in many cultures and time periods
Most Egyptians, Babylonians, and Hebrews breast-fed their children for about three years, but richer Greeks and Romans used slaves as wet nurses.
The authors discuss the topic of wet nurses in detail and give an overview of practices in many cultures and time periods.
The authors also include the story of the wet nurse Judith Waterford, who in 1831 at the age of 81 proudly showed that she could still produce milk that was of the same quality as milk produced by younger women. When Waterford was 75, she regretted that she now only had enough milk for one child and could no longer take on two children.
Most people believe that only a woman who has just given birth to a child can breast-feed.
Read also more about induced lactation or relaction and erotic lactation. Sometimes, no milk is visible in this period of breast pumping, but as soon as the infant latches on, the milk comes in (p. 52).

In the section titled “Surrogate feeding,” the authors provide examples of cross nursing. In this case, one woman nurses the child during the time when the other woman is at work or vice versa. Surrogate feeding is simply the practice of wet nursing, which generally involves the grandmothers. In the West, we can hardly imagine this occurring, but there are indeed passages in the bible where Naomi (also Noemi) serves as the wet nurse for her daughter-in-law Ruth’s child.
Surrogate feeding and breast milk bank programs
This method is still common today in certain parts of Africa. The authors include a quote from Margaret Mead from 1933 to show that even she had difficulty accepting such practices.
In newspapers and in the Charleston Medical Journal and Review, an article appeared in 1874 telling of how a 60-year-old woman had, as part of play, offered her breast to a child for three weeks and then was amazed to see that after this time milk appeared and even in greater quantities than in the case of the child’s own mother.
The authors describe how milk can be expressed by hand or with a variety of different types of breast pumps. They also provide information about breast milk banks, which have been and are still often found in children’s hospitals. This milk can be cooled, but shouldn’t be heated. Sweden and Denmark are examples of countries that have active breast milk bank programs. The banks accept milk that women produce within the first three or four months of lactation and pay a good price for this.
Eastern European countries have had an even stronger tradition. For example, 200'000 liters of breast milk were collected in the eastern part of Germany in 1989. In contrast, there are or were eight breast milk banks in the United States and one in Canada. But this milk is pasteurized in order to make sure there is no risk of contracting HIV or hepatitis.

A list of current milk banks in North America shows three for Canada, 19 for the United States, and seven that are currently in planning. See hmbana.org/locations.
When Finland began to pasteurize the milk in its banks, they found that the infection rates in infants increased and were ultimately higher than what they had been with nonpasteurized milk. Canada closed down all of its milk banks, and this turned out to be worse for the children than introducing pasteurization (p. 57).
The authors finally deal with the topic of giving infants and children the milk of another animal. In this section, they include a statement made by the Greek historian Herodotus of Halicarnassus in the fifth century BCE in which he describes how the Massagetae (in the book Massagetai) of the Caucasus, who were referred to as barbarians (galaktopotes), drank milk directly from animals: They sow no crops but live on livestock and fish, which they get in abundance from the river Araxes; moreover, they are drinkers of milk!
(p. 57)
Later, animals were used to feed infants directly, when necessary, and goats were a favorite choice as they even accepted the infant and searched for it at feeding times.
Infants in orphanages and other facilities who did not have a very high chance of survival.
In 1775, Alphonse Le Roy institutionalized the practice of feeding foundlings (child abandonment) directly from the teats of goats.
In rare instances, the infants also drank directly from the teats of donkeys.
However, it was soon realized that the life expectancy of the infants receiving this milk was much lower and that the process often led to their death. This information comes from G. J. Witkowski, "Histoire des Accouchements chez Tous les Peoples", Paris: Steinheil 1887.
Human–animal breastfeeding
But even today, some bedouins let their babies drink from goats or sheep in such cases.
More about human–animal breastfeeding. This and the opposite have been practiced for thousands of years.
And conversely, women have also breast-fed animals: Animals have been nursed by women for a variety of reasons, including to aid destitute animals, to relieve engorged breasts, to prevent conception, to promote lactation, and to develop ‘good nipples’—to name a few
(p. 59).
The authors provide examples from a number of countries, in particular, with dogs and pigs.
There are also numerous examples of women nursing the sick, aged, and imprisoned. The authors provide several examples of this found in literature. They then discuss the healing qualities of milk, in particular, for treating eye infections. Here they draw on the medical document Ebers Papyrus from about 1'500 BCE.
The healing qualities of milk
One of the most famous ophthalmologists from the middle ages, Ali Ibn Isa, also described the healing properties of breast milk around the year 1'000 CE.
In his work, he mentions ophthalmia neonatorum, which is also called neonatal conjunctivitis. This is an infectious inflammation of the conjunctiva (conjunctivitis). Ali Ibn Isa’s main work is called Kitab Tadkirat al-Kahhalin; in it, he describes 130 eye diseases.
The authors describe various other ways in which breast milk has been used to treat diseases in countries around the world.
For example, in Samoa it was used to treat a viral epidemic of acute hemorrhagic conjunctivitis.
In 1982, The Centers for Disease Control published the successful results of this old folk remedy.
The chapter ends by describing how breast milk has most recently been used to successfully treat IgA deficiencies in liver transplant recipients (Merhav H.J., Wright H., Mieles L.A., and Van Thiel D.H. 1995). Human breast milk is a rich source of IgA, which can successfully prevent enteric infections (gastroenteritis) and microbial translocation.
Section 2: Breastmilk: The Miracle Food and Medicine
This section also has two parts. Each part includes a number of topics:
Part 3 (here 2.3):
Cow’s Milk Is for Cows; Breastmilk is Species Specific; The Breasts and Milk Production; Breastmilk Is Alive; Breastmilk Components and Nipple Confusion; Breastmilk and the Premature Infant; The Fight against Infection; Breastfeeding Benefits for the Mother; Isn’t Formula Just a Third-World Issue?; The Breasts and Contraception; Is Mother’s Milk Always Safe?; Is Cow’s Milk Always Safe?; Is Formula Always Safe?; Is Bottled Water Always Safe?; Lactation-Suppressing Drugs; Adding up the Pieces
Part 4 (here 2.4):
Artificial Feeding; Infants Die like Flies; Clean Milk; Education and Advertising; The "Growing" of Artificial Foods; Feeding Vessels; Bottle-Feeding and the Environment
2.3. “Cow's Milk Is for Cows”
Professor Naomi Baumslag begins this section with the sentence Breastmilk is inimitable
(p. 67).
In the 1980s alone, more than a thousand scientific papers were published on the biochemical properties of breast milk. But even decades later, new substances contained in breast milk such as polysaccharides, amino acids, and taurines are still being discovered. At the time this book was published, and perhaps even still today, we did not entirely understand why the iron and zinc in breast milk is better absorbed (p. 67).
Even in principle, the milk of each species is different and is designed to achieve different "growthrates". This table from the book shows the days it takes for the various specious to double their birth weight and the percent content of fat, protein, and lactose (energy sources) in the milk.
| Species | Days | Fat | Protein | Lactose |
| Human | 90–180 | 3.8 | 0.9 | 7.0 |
| Horse | 60 | 1.9 | 2.5 | 6.2 |
| Cow | 47 | 3.7 | 3.4 | 4.6 |
| Reindeer | 30 | 16.9 | 11.5 | 2.8 |
| Goat | 19 | 4.5 | 2.9 | 4.1 |
| Sheep | 10 | 7.4 | 5.5 | 4.8 |
| Source: L. Hambreus, Pediatric Clinics of North America (Philadelphia: W. B. Saunders Co., 1977) 24:17. |
In the book, it lists only 180 under the days it takes for a human to double their birth weight. I added 90 days, which is now also possible because infants frequently receive cow’s milk or dairy products during the breast-feeding period.
We have gotten used to an unnaturally quick "growthrate"
The hormones contained in these can accelerate the child’s "growing" in an unnatural manner.
The German Wikipedia entry for infants states the following: After three to five months, healthy infants will have doubled their birth weight and have grown about 6 inches (15 centimeters).
In other words, we have gotten used to an unnaturally quick "growthrate" and find it to be abnormal when a child grows at the rate that nature planned!
In 1799, the physician Michael Underwood (1736–1820) compared these differences in his "Treatise on Diseases of Children" (treatise) and showed that mare’s milk is chemically closest to human breast milk and therefore a better replacement product than cow’s milk.
At the time, other major differences such as in the case of "growthhormones" were not yet known.
In addition, breast milk adapts to the changing needs of infants as they grow (EE: and likely also to their genetically determined needs).
On page 69, there is a table from F. Savage King, "Helping Mothers to Breastfeed", African Medical and Research Foundation, (Nairobi, Kenya: 1993) that provides a good overview of reasons why it can potentially be very harmful to give a baby cow’s milk instead of breast milk.
The table first shows that bacterial contamination can occur when a baby isn’t breast-fed directly. Each species drinks directly from the nipples or teats of the udder. They also get the antibodies and leucocytes they need, which aren’t present in formula or milk from other animals. In addition, breast milk supplies the baby with lactoferrin and bifidus factor.
Why it can potentially be very harmful to give a baby cow’s milk instead of breast milk

Researchers first isolated N-Acetylglucosamine from the protein-free fraction in breast milk. However, today we know that the bifidogenic effect of breast milk is not based on any single factor, but rather on the complex interaction of numerous substances. These include oligosaccharides, high lactose levels, low protein levels, antimicrobial proteins such as lysozyme and lactoferrin, and specific sIgA antibodies that work against the accompanying flora.
For healthy brain "growing", babies also need the special amino acids found in breast milk such as cystine, taurine, and linoleic acid. Breast milk also contains many more important unsaturated fatty acids and fewer “bad” saturated fatty acids than cow’s milk. In addition, cow’s milk doesn’t contain lipases, which are important for the digestion of fat.
Cow’s milk includes far too much sodium, chloride, and potassium with levels that are at least double to triple what they should be. And babies get four times more calcium and six times more phosphates than their bodies are prepared for.
Bioavailability also plays a role. For example, cow’s milk contains more iron than breast milk, but infants only absorb 10 % of this iron, whereas they absorb 49 % of the iron in breast milk.
Baumslag writes, If every newborn in the United States were breastfed for just twelve weeks, the health care savings from avoiding nonchronic diseases in the babies’ first year of life would amount to $2–4 billion annually
(p. 70).
When a baby drinks breast milk, it is getting the right vitamins in the right amount and enough water. The authors calculate that the illnesses related to formula cost a total of $333 billion annually.
The authors explain that having small breasts is no reason to worry. The size of the breast is determined by the fat cells, which are either present in the body to a smaller or greater extent. The milk ducts are not affected.
However, if a mother is malnourished, the fat reserves can help her to produce enough milk.
Next, they describe the various organs involved in milk production and lactation. We learn some about the circuit that allows the milk to come in and flow, and about some of the reasons why this process is sometimes blocked.
Foremilk and hindmilk
When a mother breast-feeds her child, the milk the baby drinks at the beginning is called foremilk and the milk at the end hindmilk. These two types of milk are quite different and it is important that the baby receives a good balance of foremilk and hindmilk.
The foremilk is significantly lighter in color and not as yellow as the hindmilk.
These include "oxyto.." ("pitoc..") and ergot (product: "Methergi.." from Novartis), which was previously used to stop uterine bleeding.
A mother who is breast-feeding shouldn’t clean her nipples with alcohol because the baby may then not “acquire the taste” (olfaction). And for this reason, they shouldn’t rub their breasts with a coarse washcloth or apply lanolin (wool wax) or other oils even though this is a recommended standard practice in many hospitals.

During the breast-feeding period, lanolin is also used to help with cracked nipples. When washing, you should go around the nipples and aerola, avoiding this area. And you should only touch your breasts after you wash your hands with a mild soap.
According to Wikipedia, mothers should leave the last bit of milk on their nipples as this helps to prevent drying out. It also has an antibacterial effect and helps prevent cracked nipples.
Dr. Baumslag describes the entire process of milk production and the stimuli required. She also discusses the various organs involved, but that is not of central importance for our task at hand, which is why I chose not to include this part.
The smell of the breast is important for infants. For example, newborns can find the breast with their eyes closed. They simply follow the direction of the smell of the excreted, protective sebum.
A problem with bottles is that babies don’t have to work for their milk, and they are then full before they have had opportunity to satisfy their oral and touching needs. Incidentally, a woman who has never been pregnant can also give milk. For this, the preparations described above are necessary.
Bottle-fed babies more often develop the habit of thumb-sucking than do breast-fed babies (p. 73). According to Wikipedia, thumb-sucking is a way for children to comfort themselves.
Dr. Baumslag has titled the next section Breastmilk is alive
; here she covers the substances contained in breast milk and colostrum. Colostrum, or the first milk produced, is called “liquid gold” because of its color and importance for the child. It is a sticky yellow substance that contains many important antibodies, proteins, white blood cells, and carotene, as well as vitamins A, B12, D, E, zinc, and other substances. This milk changes gradually in the first few days to transitional milk and then to mature breast milk, which adapts to the babies’ needs.
Colostrum and Meconium
Colostrum has a lower nutrient density than mature breast milk, but this allows babies to first build up their antibodies and have their first bowel movement, which is mostly the excretion of blackish green meconium.
As a result, babies usually lose about 10 % of their weight at the beginning. Meconium, unlike feces, does not contain food.
 | A newborn normally excretes meconium only in the first 24 to 48 hours. Meconium is not a digestive end product (feces or stool). Instead it is a dark viscous substance that collects in the intestine, which is not yet functioning. Meconium is made up of the desquamated epithelial cells of the mucous membranes, thickened bile, and hair and skin cells swallowed along with the amniotic fluid. |
Meconium aspiration syndrome (MAS) can be life-threatening for an infant. But MAS is rare even though 13 % of all newborns enter the world in amniotic fluid containing meconium. Only 5–12 % of these newborns develop MAS. Extracorporeal membrane oxygenation (ECMO) or extracorporeal life support (ECLS) is only necessary in very difficult cases.
Professor Baumslag explains that there are many contradictory studies on colostrum and unnatural supplementary foods. This stems from the fact that an infant who is breast-fed only once a day and then given formula is still statistically considered to be a breast-fed infant, which is a big mistake. Some studies adopt this definition, whereas others define breast-fed infants as those babies who are exclusively breast-fed.
Mortality rate of infants
Next there is a table from 1987 that shows how the mortality rate of infants in developing countries increases dramatically when they are not breast-fed exclusively. This holds true in spite of the use of modern medicine.
When a woman has a preterm birth, her breast milk is different than that of a mother who gives birth between weeks 37 and 40 of the pregnancy. Breast milk is alive and changes to meet the needs of the baby.
The authors include a convincing list showing the benefits that breast-feeding has for babies (15) and mothers (12) and the disadvantages that it has for artificially fed babies (7).
Diarrhea, gastrointestinal illnesses, and urinary infections, in particular, are less common. The same holds true for respiratory diseases, ear infections, allergies, and sudden infant death syndrome (SIDS).
According to the statistics, breast-fed babies also have fewer problems with learning and behavioral difficulties and show better psychological development.
They develop
a more energy-efficient and rhythmically functioning nervous systemandare less likely to develop heart disease and cancer later in life(p. 78).
The authors then list out many benefits of breast-feeding and the disadvantages for babies that receive a combination of breast milk and formula or are artificially fed (p. 78).

Today, the risk of becoming obese is higher than ever. As compared to breast-fed babies, bottle-fed babies are at least three times more likely to develop adult obesity (p. 78).
The reasons behind the disadvantages listed of giving a baby formula as compared to breast-feeding
A breast-fed baby gets enough liquid, which you can be sure of if the baby has soft stools and enough wet diapers (6–8 per day).
Studies in India and Honduras have shown that even breast-fed babies in these hot climates receive enough fluids. The reason for this is that the babies are fed on demand, whereas formula-fed babies have to wait three hours until they have digested the artificial milk.
This can lead to a vicious circle in which the baby no longer uses the proper sucking techniques and virtually loses its appetite, and as a result the mother produces less milk (lactation) (p. 81).
The authors spend several pages explaining the reasons behind the disadvantages listed of giving a baby formula as compared to breast-feeding. Then they provide reasons as to why breast milk is perfect and information about the substances contained in breast milk. Certain substances are also found in cow’s milk, but the amount and quality of these are ideal for calves, not humans.
The anti-infective components of breast milk include the following anti-infectious factors: bifidus (bifidobacterium), secretory form (dimer) of Immunoglobin A (IgA) and IgG or gamma globin (The book incorrectly lists IgC here; see also immunoglobin superfamily), antistaphylococcus factor (staphylococcus), lactoferrin, lactoperoxidase (LPO), complement C3 and C4 (complement system), "interferons" (IFN), lysozyme (muramidase), B12 binding protein (see transcobalamin and haptocorrin), lymphocytes, and macrophages (scavenger cells and MΦ).
Dr. Baumslag explains why it is so important that preemies receive the breast milk that is specifically tailored to their needs and development phase.
The breast milk helps, for example, to protect their intestine. The Australian reproductive biologist and cell biologist Dr. Roger Valentine Short writes why the feces of a baby who is exclusively breast-fed don’t smell “unpleasant” to the mother. He shows how primates can develop specific antibodies (IgA) just by consuming even the smallest amount of the infants’ feces. The IgA in the breast milk then helps to protect the child (p. 90).
Breast-feeding also has very positive benefits for the mother.
It helps contract the uterus, mothers lose the pregnancy weight more quickly and are able to get back in shape, and they feel more relaxed and happy.
There are certain groups that try to make the public believe that the negative effects of formula milk, as compared to breast milk, only apply to developing countries.
It is true that the use of formula results in much greater negative effects in these countries than in industrialized countries. But it has been shown that breast-feeding has extensive medical benefits, in all places, at all times, and for all women
(p. 93) — and today there is no way that we can deny the existence and logic of these scientific results.
Dr. Baumslag strengthens her arguments by providing statistics from 1981, 1989, and 1992. In this period, bottle-fed babies had gastrointestinal illnesses five times as often as breast-fed infants.

For fans of logic: by listing out the ways that breast milk is tailored to babies, this book shows how breast-feeding is highly superior to all artificial means of feeding babies. But it is a futile battle (almost) to try to change the current situation with just a few books and articles. How could this be enough in light of the huge budgets of multinational companies and the influence they have on politics and media? It is similar to the struggle of Don Quixote, in the novel written by Miguel de Cervantes.
In a section on contraception, the authors quote Aristoteles, who wrote in 350 BCE that menstruation doesn’t occur during breast-feeding and that a women’s milk will dry up after she conceives. This is generally true, but there are some exceptions. (p. 93)
We then learn that breast milk can be harmful if, for example, the mother is consuming alcohol, tobacco, or drugs. Exposure to chemical toxins or lead-contaminated soils can also make breast milk unsafe. This information is used by certain groups to discourage mothers from breast-feeding; however, these factors are primarily harmful during pregnancy.
If a mother has an infection, she should not give up on breast-feeding because her antibodies protect the baby; in fact, the baby is more likely to get the infection if the mother stops breast-feeding. With infections, the main route of infection is via the skin, and also secretions from the mouth and nose, and not via the milk (p. 98).
Radical diets, radioactive iodine, acohol, drugs, HIV and reasons to stop or take a break from breast-feeding
Women should avoid radical diets when they are pregnant and breast-feeding. When fat is released (as a result of dieting or starving oneself), the fat-soluble toxins stored there enter the bloodstream and also the breast milk. These toxins include substances such as polychlorinated biphenyls (PCBs), heptachlor, and dioxins. Furan, used as a flavor enhancer in coffee, can also accumulate in fat tissue.
A Swedish study showed that after the nuclear accident in Chernobyl, the cow’s milk in Italy and Austria contained 300 times more radioactive iodine and cesium than the breast milk.
But thanks to the "oxytoc.." that is produced during breast-feeding, mothers have less need for these types of drugs and focus more on the needs of their babies than mothers who give their babies formula.
There are very few good reasons to stop or take a break from breast-feeding. However, if the mother is going to have chemotherapy or treatments with radioactive compounds or gets food poisoning, she should do so. If radioactive iodine is used in a diagnostic exam, the mother should stop breast-feeding for 24 hours.
In the case of a herpes sore (herpes simplex) on the nipple or aerola, the mother should only breast-feed with the other breast. If a small infant is infected with herpes, it can lead to very serious problems.

Neonatal herpes simplex, the HSV infection in newborns, is very rare. The disease can be transmitted during birth if the mother has herpes genitalis and is then very dangerous. However, this is not at all related to a herpes sore on the breast.
If a mother or father (or other family member or friend) has herpes in the mouth area, they shouldn’t kiss the child if there are any blisters or scabs around their lips.
It is important to always wash your hands thoroughly before you touch a child. Before breast-feeding, a mother should always inspect her breasts. Cosleeping is dangerous in this case?
According to experts from the Centers for Disease Control (CDC), WHO, and UNICEF, even in the case of an HIV infection, the death rate of babies is higher if they don’t receive breast milk. This doesn’t apply to conditions and areas where child mortality is low. It is a known fact that breast-fed children who are HIV positive develop AIDS later than do formula-fed children (p. 100).
On the next few pages, we read why cow’s milk offers much less security when it comes to contamination. For example, in 1989 the Wall Street Journal found that 38 % of 50 milk samples from ten cities contained antibiotics and sulfa drugs (sulfanomide).
The milk is fortified with certain substances, which can also cause major problems.
Vitamin D intoxication
In 1990, physicians were alarmed because a 15-month-old child and a 72-year-old woman were suffering from Vitamin D intoxication (cholecalciferol).
The milk from the dairy was analyzed, and it contained up to 914 % more Vitamin D than is standard.
And then eight more people in Massachusetts also got sick from consuming too much Vitamin D.
It was discovered that the milk they drank contained anywhere from absolutely no Vitamin D up to 500 times the recommended amount.
Formula milk that was tested at the time contained up to 4.5 times more Vitamin D than stated on the label.
 | Cholecalciferol, which is physiologically present in all people, or rather in all living creatures with cells containing a nucleus (eukaryotes), is called vitamin D3. Since cholecalciferol is produced in the skin from 7-dehydrocholesterol, with the help of UVB radiation (previously called Dorno radiation), it is actually a prohormone and not a vitamin. A vitamin D deficiency can cause rickets in children and osteomalacia in adults.
|
Wikipedia (German entry): Fortifying everyday foods with vitamin D is currently prohibited in Germany because of the toxicity of vitamin D. Since butter has a high level of vitamin D naturally, manufacturers have special permission to add vitamin D to margarine so that they can make it similar to the original product.

Note: Consuming too much vitamin D can lead to the occurrence of schizophrenia, seizures, and liver damage. Small children reach the toxicity level much more quickly than adults. If certain conditions are met, sunlight is the best source of vitamin D.
Dr. Baumslag also explains the problem of regularly giving cows artificial "growthhormones". This brings about 10 to 30 % higher milk yields; however, the cows suffer from mastitis more often and have to be treated with antibiotics. Many additional problems also occur.
Monsanto developed the "growthhormone" rBGH, which is present in the cow’s milk in the countries involved. In Europe this is (still?) prohibited. You can read more about rBGH and IGF-1 in this book review of "Milk, The Deadly Poison".
"GrowthHormone" rBGH, "InsulinGrowthFactor" and cancer
The rBGH in cow’s milk causes the production of more "InsulinGrowthFactor" (IGF-1). And IGF-1 promotes the progression and malignancy of breast cancer, as well as the spread of cancer into other tissues (metastasis). Newsweek magazine called this “a medical disaster” (p. 102).

EE: I call this the accelerator for cancer. While physicians are hitting the breaks, patients are consuming more dairy products and with these more "growthhormones".
But between 1982 and 1994, the food industry had to recall formula in 22 different instances as the formula was not safe. A large majority of these cases could cause death or lead to serious or irreversible health problems for the babies.
In appendix C on pages 223 to 226, you can find a list of these formula recalls with a description of the problem in each case. Only six of these 22 products were classified as not likely to cause medically adverse health effects
(p. 224). The information comes from the FDA and applies only to the United States.
Some of the problems, formula in developing countries and mistakes made in the preparation and storage of formula
Here I will only list out some of the problems:
- klebsiella contaminants (which can cause respiratory and urinary tract infections),
- salmonella contamination (which can lead to serious infections),
- glass contamination (2 instances),
- general bacterial contamination,
- toxic vitamin A levels,
- and deficient levels of vitamin D, folic acid (vitamin B9), zinc, copper, linoleic acid, vitamin B6, and thiamine (vitamin B1).
The authors then describe instances of problems with formula in developing countries. But similar problems have also occurred in the U.S., and in this time entire factories had to shut down as the problems were so serious.

Wikipedia explains a case in New Zealand in the entry titled the 2013 Fonterra recall.
Fonterra sold about 1'000 tons of whey contaminated with bacteria to companies that produce formula and sports drinks. The products were then exported to seven different countries.
The Ministry for Primary Industries brought attention to the case and announced the recall. Although the discovery was made much too late, the company was lucky because the strain of clostridium bacteria turned out not to be toxic.
The case does however show that we can’t claim that incidences like those described in the book are no longer possible.
On Wikipedia, you can go to the entry on infant formula to read more about the problems with artificial milk. The good news is that the nutritional information in this entry is presented in a fairly neutral manner. You will find many aspects that verify the information in this book.
A wide range of mistakes are made in the preparation and storage of formula. Low water quality, such as too much lead in the water, can also play a role.
In the United States, very high levels of lead are often found in the drinking water. And many parents, and babysitters and grandparents, add more formula to the water than is recommended because they believe that this will only help the child. However, this practice has caused death in multiple cases (p. 104).
The authors warn readers not to use bottled water. Breast-fed children don’t need bottled water, and in most cases it is better to give bottle-fed children formula mixed with tap water. The reason for this is that babies can experience water intoxication if they are given formula mixed with bottled water. Water intoxication is an imbalance of the water electrolytes in the body that occurs in cases of overhydration.
Using drugs to suppress lactation?
Under the term lactation suppression, you will find a Wikipedia entry describing the problems that arise if a woman wants to terminate lactation right from the start. It is interesting that there doesn’t seem to a similar entry on the German Wikipedia site.
Dr. Baumslag also explains that women can have a large amount of pain when the milk comes in and is then not expressed. Fortunately, drugs are no longer recommended to stop lactation.
The side effects of such mediations are well documented. If a newborn dies or has to be given away, the woman has a problem. An FDA study showed that 90 % of women did not have pain strong enough to make them need to take pain relievers. And the most painful period lasted only for about 12 hours. The pain then resides, and the milk dries up within 10 days.
Lactation-suppressing drugs
Since 1989, "bromocripti.." ("Parlod.." from Sandoz, possibly also Pravidel, Kirim, and Umprel) has been the only drug that is approved in the United States after other drugs caused numerous cases of serious complications and several deaths.
But promocriptine (from Avenzor), a "dopamineagonist" only available as a prescription, has also caused 13 deaths and a number of health problems in the United States (p. 106).
In 1994, the FDA was forced to withdraw the approval of "bromocripti.." as a lactation-suppressing drug. "Parlod.." is now labeled only as a medication to treat Parkinson’s disease, but physicians have the right to prescribe any drug that is approved.
Disheartened, the authors write: It would be easy to blame the women for being so selfish that they would endanger their health rather than let their own child suckle from their breast. But the FDA, the medical profession, and the drug makers are the real culprits. What kind of society have we created that will direct so many resources at stopping lactation—and so few at encouraging it? (p.108)
After World War II, many American women changed over to bottle-feeding their newborns. Between 1946 and 1956, the previously high rate of breast-feeding fell to 25 %. And as a result 25 % of the babies received formula and 50 % were given evaporated milk.
In the 1990s, over 50 % of American women still chose not to breast-feed
EE: Borden introduced milk in bottles in 1885 and began selling evaporated milk in 1892.
 | Evaporated milk is dehydrated milk from which about 60% of the water has been removed. It can be stored at room temperature for months, or even years, and only takes up half the room that milk does. This homogenized and sterilized milk is sold in tin cans. It can’t be compared with condensed milk (usually sweetened to allow for longer storage) or powdered milk. |
In the 1990s, over 50 % of American women still chose not to breast-feed. Only one in five children is still being breast-fed after the age of five months. Even though the numbers have improved, it has primarily been more educated and affluent women who have accounted for this change.
The practice of bottle-feeding has increased drastically in many developing countries. Between 1986 and 1989, the percentage of infants in developing countries who were exclusively breast-fed during the first four months was as follows: Nigeria (1%), Ghana (2%), Brazil (3%), Thailand (4%), Senegal (6%), Mali and Togo (8%), and Zimbabwe (9%).
However, there have been some successes. For example, in 1989 Dr. Natividad Relucio-Clavano introduced exclusive breast-feeding and rooming-in in her hospital in the Philippines and achieved a significant decrease in infant mortality. And the hospital costs were dramatically reduced because the infants were not sick as often. This led to a general trend away from bottle-feeding in the Philippines.
In 1986, a hospital in Quito, Ecuador, with 14 thousand births per year also decided to cease all use of formula and, as a result, achieved a dramatic decrease in newborn infections and infant mortality.
Infant mortality at Baguio General Hospital decreased by 95%
| Dr. Natividad Relucio-Clavano (1932–2007) began her program in 1973 and published astonishing results in 1977. Read more general information here and more about her last victory. According to this good-bye by UNICEF, infant mortality at Baguio General Hospital decreased by 95% thanks to her efforts. Professor David Morley, a British pediatrician lists her as his only “notable student.” |
2.4. Artificial Feeding
The section "Infants Die Like Flies" begins somewhat like a crime novel. The events are as terrible as the fact that starting in 1847 Dr. Ignaz Semmelweis worked with no success to introduce mandatory handwashing for physicians before operations and births. At the time, physicians sometimes dissected corpses before delivering babies.
But even breast-fed infants had a high mortality rate. Even worse, between 1775 and 1796 in the foundling hospital in Dublin, the mortality rate was 99.6 %. Of a total of 10'272 children, only 45 survived.
Relevant statistics
The authors include some relevant statistics. For example, in the mid-1760s in London, there was an average of 16'283 births per year, and 7'987 children under two died. An additional 26 % died before they turned five.
The British businessman and philanthropist Thomas Coram (1668–1751) worked for twenty years to open an institution that would take in foundlings so that they literally would not have to rot on dung heaps. In 1745, he was finally able to open Foundling Hospital, the first foundling hospital in the world for children who had been abandoned by their parents. Thomas Coram died destitute soon thereafter.
Since it wasn’t possible to give the infants breast milk, the foundling home had a death rate of two-thirds. Of the 15'000 infants in the home, 10'000 died. However, in certain parts of London, the death rate was as high as 80–90 %.
This horrendous mortality rate is included in the article Breastfeeding, Fertility and "Populationgrowth" by Roger Short, in the ACC/SCN Symposium Report, UNICEF, August 1993.
A century later, in the nineteenth century, the infant death rate was still 40 %.
In southern France, Monsignor Morel, the mayor of Villiers-le-Duc, reduced the mortality rate of infants under one year from 30 % to 20 % between 1852 and 1854. He did this by giving the parents a generous monetary award if their child lived to celebrate its first birthday.
Starting in 1893, Morel’s son had all of the babies weighed every two weeks by a physician and made sure that the babies only received breast milk. The program was so successful that between 1893 and 1903 not a single infant died.
Milk stations, chlorination of drinking water, better methods of sewage disposal and pasteurization
At about the same time, the obstetrician Pierre-Constant Budin (1846–1907) introduced milk stations where the infants were weighed and given sterilized milk if their weight gain was not satisfactory.
In 1880, both chlorination of drinking water and better methods of sewage disposal were introduced. There were also new regulations to ensure healthier dairy herd housing and feeding.
The authors describe the miserable conditions in the dark stalls where the cows were kept. They often had typhus, tubercolosis, skin problems, and other diseases. Sometimes they were so weak that they had to be hoisted up before they could be milked (image: Harper's Weekly, May 15, 1858).
The storage, transport, and treatment of the milk also improved. For example, Louis Pasteur (1822–1895) developed the process of pasteurization. All of these measures contributed to the fact that the life expectancy of bottle-fed children gradually improved (p. 117).
However, a study from 1985 conducted in an urban area in southern Brazil showed that bottle-fed children died of diarrhea 14 times more often than breast-fed children (p. 113–114).
In 1991, there were eight deaths per thousand live births in industrialized countries, whereas two to four percent of the infants (84 to 188) in developing countries still died. The major cause was and still is diarrhea that can’t even be cured with modern hygiene and medicine.
The Semmelweis reflex
After birth or miscarriage, the uterus is like a large wound surface. The cervix is still widely open in the days following the birth. This makes for a direct connection between the uterus and vagina, and absolute hygiene is necessary.
Vaginal discharge (lochia) after birth and previously margination (macrophages) beforehand help to naturally prevent infections. When the mother breast-feeds, she produces "oxytoc..", which supports this process.
In 1843, Oliver Wendell Holmes argued that physicians also transmit diseases. Dr. Semmelweis then introduced hygienic practices in his department. This effectively prevented puerperal infections (postpartum infections, puerperal fever, or childbed fever). When he tried to convince his colleagues to do the same, Dr. Semmelweis (not Semmelweiss) was ridiculed by his colleagues for over 20 years. He died in an asylum at age 47. An attendant beat him to death.
Joseph Lister was the first physician to introduce effective hygienic practices based on findings made by Louis Pasteur (and Casimir Davaine, 1863). Physicians in German-speaking countries followed suit five years later.
This is at least very true in the case of baby food, milk, and dairy products.
In 1867, Justus von Liebig (1803–1873) developed the first formula and called it the “perfect food” (p. 120). The ingredients in his formula were cow’s milk, flour potassium bicarbonate (potassium hydrogen carbonate), and malt.
Many physicians felt that this formula wasn’t suitable for infants, which very much annoyed von Liebig. He therefore developed new types of formula, including a formula based on condensed milk.
Powdered milk and refrigerators
| The Russian physician Osip Krichevsky developed powdered milk in 1802. William Newton developed and patented sweetened condensed milk (SCM) in 1835 (1837), after Nicolas Appert (1749–1841) made condensed milk in 1922. Tin cans were introduced in 1810 by Peter Durand and then commercially produced by Bryan Donkin and John Hall starting in 1813. |
Appert opened a food bottling factory in 1804 and used Durand’s tinplate cans starting in 1812. In 1856, Gail Borden patented the industrial production of condensed milk, and starting in 1866 Nestlé marketed condensed milk in tin cans. John B. Meyenberg developed dehydrated milk without added sugar, and starting in 1885 he used his process at the Helvetia Milk Condensing Company.
Refrigerators didn’t become common until after World War II. Although one in two households in the United States had a refrigerator in 1937, they weren’t introduced to the general public in Europe until after the war. Refrigerators made it possible for people to store the milk for a few hours or even a few days.

Information about refrigerators (previously iceboxes): In 1748, William Cullen gave the first demonstrations of artificial refrigeration. Starting in 1834, these systems were commercially marketed by Alexander Twinning. And In 1859 Ferdinand Carré used gaseous ammonia dissolved in water to develop a gas absorption refrigeration system.
You can basically say that since the twentieth century it has been well known that breast milk is absolutely the best food for a baby. And by that time, the hygienic practices were better so that milk, dehydrated milk, and condensed milk caused fewer problems than had previously been the case.
And in the cities, there were actually milk stations that provided milk to mothers who couldn’t breast feed, weighing programs for infants, instruction in the best way to feed and care for infants, and access to specialists.
Educational programs and a significant decrease in the infant mortality rate
Some of the “milk depots” offered bottled milk free of charge to the needy, for example, the stations owned by the philanthropist Nathan Straus (1848–1931), (not Strauss as is listed in the book) in New York (p. 122).
Some of these milk stations were later turned into clinics that recommended breast-feeding. Nurses, doctors, and other public health officials made home visits as a way to improve the health of children.
Dr. Sara Josephine Baker (1873–1945) showed in 1908 that these visits were responsible for a significant decrease in the infant mortality rate.
She started “the little mother leagues,” which was a program that provided young girls with practical information about birth, breast-feeding, and childcare, and in which they served as “missionaries” to spread this important information. In poorer families, in particular, if the mother worked, girls in the family often took care of the household.
England had the Truby King program, which was started by Sir Frederic Truby King (1858–1938). In this program, nurses provided families with advice on how to best care for their infant. King also emphasized the importance of breast milk, but he advocated the undesirable practice of nursing babies every four hours instead of on demand. Most of the women either didn’t have a clock or didn’t understand how to use the clock (Rapport 1925) (pp. 28 and 125).
People thought that nursing at irregular times was the reason for “summer complaint” (summer diarrhea, not Shigella), which in the United States occurred primarily in cities. The disease was very common in children between the ages of 4 and 20 months and was often fatal. Mothers followed this program and chose to let their children cry rather than nurse them on demand.
The pediatrician Dr. Preston Alexander McLendon (1893–1980) and psychologist and new mother Dr. Frances Parsons Simsarian (1912–2005) are to thank for the fact that women were again encouraged to feed their babies on demand and not according to the clock.
In 1942, Dr. Simsarian nursed her baby when it seemed hungry and after a few days it was calmer and adapted to a schedule of breast-feeding six or seven times a day.
Dr. Benjamin McLane Spock (1903–1998), pediatrician and psychiatrist, included information about this experiment in his book "Baby and Child Care" in 1946. Before he died, fifty million copies of the book had been sold.
Kathleen Auerbach was a leading figure in La Leche Liga (LLL), which was founded in the United States in 1956. Today, the LLL is integrated into the LLLI, which stands for LLL International.
LLL consultants are mothers who have nursed their own children and completed training to become LLL lactation consultants. They support parents during the nursing period and offer help with breast-feeding, when there are difficulties or uncertainty about certain aspects. This can take place via telephone, email, or personally in a breast-feeding group. The consultation is free as the consultants work on a volunteer basis. The organization is funded by donations and membership fees.
The LLL supports attachment parenting, which was developed by William Sears. LLL is the most important organization that works to provide mothers with information and support about breast-feeding. Contact information can be found here. First select your country.
Professor G. J. Ebrahim (1932–2012) from the Institute of Child Health (UCL) in London showed how the child welfare clinics were increasingly becoming the best customers and advocates of artificial milk. However, this had started much earlier. For example, the American Condensed Milk Company appealed to mothers as early as 1865 with the slogan Safest milk for infants and children
(p. 127).
The "safest milk for infants and children" again led to high child mortality rates
This safest milk for infants and children
again led to high child mortality rates. At the time, it was already common to quote physicians in advertisements.
And then later came statements from Nestlé such as indispensable as a diet for infants
(p. 127). In 1873, Nestlé sold a half a million boxes of “farine lactée.”
The manufacturers of this baby formula knew that this milk was not near to being able to meet the needs of infants. The formula was therefore continually changed over the next century. The changes were naturally made to improve the formula, but also to save on costs.
The book author Kathleen G. Auerbach wrote the following in the Journal of Tropical Pediatrics in 1992:
The formulations for artificial baby milk are changed frequently and represent one of the largest uncontrolled experiments in altered nutrition for humankind ever conducted (p. 127).
The authors report on the excessive marketing campaigns, which were a lucrative business for physicians, some of whom owned factories themselves.
It was seen as ‘men of sense’ rather than ‘foolish unlearned women,’ taking over the supervision of infant care
(pp. 129–130).
And indeed the industry successfully introduced baby formula into developing countries on a large scale and caused the death of a huge number of children there.
Feeding bottles, "nursing attachments"
The book explains how the many different baby formulas available often contain widely differing ingredients. In the middle of the 1990s, this industry had annual revenues of eight billion dollars.
On the following pages, we learn about the different types of feeding bottles used from 1777 until 1990. At first, metal feeders of varying shapes were used. As these are only of historical interest, I will not go into further detail.
The patent for a “nursing attachment” that covered both breasts (1910) is both interesting and grotesque. It included a tube from the breast to the baby so that it would be possible to nurse in public (p. 139).
Finally, the authors explain the costs of using formula instead of breast-feeding and how waste accumulates from the production of formula.
On page 142, we learn how breast-feeding would help to reduce world population. This statement may sound paradoxical, but breast-feeding is an effective form of contraception that prevents women from having babies too close together and improves the overall health of babies. This, in turn, lowers the death rate, and women choose to have fewer babies. When the death rate is high, women have more babies as this is seen as a type of “insurance policy” (p. 142).
Breast milk is sold successfully and at high prices to bodybuilders

It’s crazy how people tick. Many babies aren’t given any breast milk, but we hear about how breast milk is sold successfully and at high prices to bodybuilders.
On June 22, 2015, the headline of the Swiss newspaper 20 Minuten read "Fitness Freaks Swear by Breast Milk" and the subtitle was "It helps you build strong muscle and is good for the regeneration phase: the milk from women’s breasts".
Experts question its effectiveness and warn of possible diseases.
It can be argued that this is better than consuming protein drinks or anabolic substances. But "growthhormones" cause all cells to grow and not just muscle cells — and cow’s milk contains higher levels of "growthhormones" anyway.
Cow’s milk also contains more protein and fewer carbohydrates than breast milk.
Section 3: Breastmilk Economics — Shaping Corporate and Governmental Policies
Part 5 (here 2.5):
The Global Search for Formula Sales; The Search for Consumers; Private Profit versus Public Health; Turning the Tide — The Era of Activism; Developing the WHO Code; The Code; The Boycott Ends ... and Begins Again; Is the Code Working?; The United States Embraces the Code; The Medical Connection; The Discharge Debate; The “Baby-Friendly” Effort is Launched; The WIC Program; Supplying WIC with Formula; How Should Formula Be Sold?; Where Are We Now?
Part 6 (here 2.6):
Women and Work; The Work of Women; A Historical Perspective of Maternity Entitlements; Breastfeeding at Work
2.5. The Global Search for Formula Sales
The authors describe how breast-milk replacement products, which often result in infant deaths, have at times been marketed as modern and fashionable. This has paid off for the industry, which earns more than eight billion dollars annually on baby formula. We learn about the steps the industry has taken to convince women that bottle-feeding is the best choice — to the detriment of their children.
From a speech given by Dr. Cicely D. Williams (1893–1992) at the Singapore Rotary Club in 1939 titled Milk and Murder:
If your lives were embittered as mine is, by seeing day after day this massacre of the innocents by unsuitable feeding, then I believe you would feel as I do that misguided propaganda on infant feeding should be punished as the most criminal form of sedition, and that these deaths should be regarded as murder. ... Anyone who, ignorantly or lightly, causes a baby to be fed on unsuitable milk, may be guilty of that child’s death.
In the nineteenth century, the focus was on researching and developing the best type of formula to replace breast milk, whereas in the twentieth century the idea was that breast milk must be replaced so that the revenues and profits would be large. Through skillful marketing and promotion campaigns along with medical complicity, (e.g., lavish conventions), artificial feeding gained both societal and medical legitimacy.
The disease called kwashiorkor, caused by insufficient protein consumption
| The pediatrician Dr. Cicely D. Williams discovered the disease called kwashiorkor and correctly described how it is caused. It was previously thought to be pellagra, a disease caused by a severe deficiency of vitamin B3. Kwashiorkor, on the other hand, is caused by insufficient protein consumption. Although she correctly described and differentiated kwashiorkor from pellagra in The Lancet in 1935, her colleagues and supervisors on the Gold Coast were hostile to her for years and ended the work with her on unfriendly terms in 1936. |
Dr. Williams was sent to Malaya to teach at the University of Singapore. She quickly recognized that she had an entirely different problem to deal with: a high child mortality rate influenced by helpers from Nestlé and other infant food manufacturers who were dressed as nurses and sent to recommend condensed milk in place of breast milk.
After spending difficult years in a Japanese prison and only nearly escaping a death sentence, Dr. Williams was appointed director of the Mother and Child Health division at the World Health Organisation (WHO) in Geneva. Wikipedia describes her story in detail. Click on her name above to read more.
Eventually the manufacturers turned to the developing countries. Their goal was that women would start using formula as soon as possible and they began their work by promoting formula in maternity wards. Free deliveries. For example, in the 1960s the United Nations International Children’s Education Fund (UNICEF) distributed large amounts of milk powder for malnourished infants, almost two million pounds each year.
This helped artificial feeding with milk powder to gain popularity in the developing countries. The interests of the dairy industry were in direct opposition to what was in the best interest of the infants as this change resulted in a high child mortality rate.
Marketing, distribution, influence and "bottle-baby disease"
In a table on page 149, the authors show the many channels used for marketing, distribution (sales logistics), and influence. And it shows how physicians, nurses, and midwives have been provided with grants, remuneration of expenses, equipment, literature, gifts, advice, recipes, free samples (product samples), brochures, and other helpful items to make promoting formula easier and more rewarding.
Hospitals received gifts and even free architectural services for the renovation of their maternity wards. The formula industry lured professional organizations with direct donations, conventions, research grants, free dinners, conferences, travel money, and other services.
The authors describe just how intense the advertising for baby formula was and how the extensive marketing worked to generate large amounts of money in the cities of developing countries.
For example, trained nurses were given commission when they convinced mothers to use formula, and the mass media was also used to reach mothers.
Previously, the quality of breast milk had never been questioned. But then all of a sudden, the slogan was: When breastmilk fails, choose Lactogen
(p. 50). People even began to believe that breast milk was inferior and that formula was something like medicine.
In just one month (August 1974) in Sierra Leone, there were 135 30-second advertisements for Lactogen (Nestlé), 66 for Similac (Abbot Labways), and 45 for Cow & Gate (Unigate).
The message was clear: sterile, scientific, superior.
You can imagine the sanitary conditions under which water was added to the formula to prepare it for the child. The term “bottle-baby disease” was coined.
After Dr. Cicely D. Williams gave her speech in 1939, it took about 25 years until the children’s specialist Dr. Derrick B. Jelliffe (1921–1992) and his wife Dr. Eleanore Florence Patrice Jelliffe (1920–2007) coined the term “commerciogenic malnutrition” and with their research drew attention to the many problems caused by bottle-feeding. The pediatrician Dr. Catherine Wennen also described the disastrous situation in Nigeria in the 1960s.
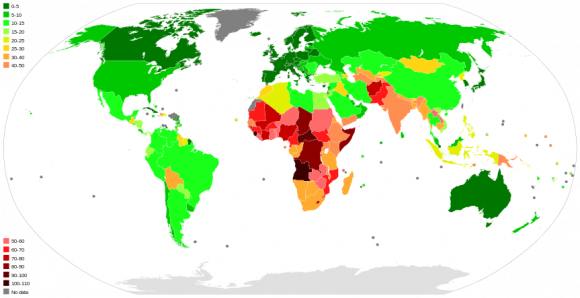
In 1968, the monograph "Infant Nutrition in the Subtropics and Tropics" was written by Derrick B. Jelliffe and published by the WHO — the couple wrote many papers and books over the course of their careers.
The Era of Activism
The collective activities of health care workers and other activists finally became visible enough that the United Nations Protein Advisory Group met in 1970 to discuss the problem.
In 1973, Drs. Puffer and Serrano in South America und Drs. Plank and Milanesi in Chile also showed the clear relationship between the more widespread use of formula and the increasingly high child mortality rates.
The clear relationship between the more widespread use of formula and the increasingly high child mortality rates

To read more about the work conducted by Plank and Milanesi, see the book "Breastfeeding and HIV/AIDS: The Research, the Politics, the Women’s Responses" written by Edith White. There you will read that mixed-feeding, as described by Stephen J Plank and Milanesi ML, was found to be connected with a slightly higher infant mortality rate (86.5 per 1'000 infants) than exclusive bottle-feeding (84.5 per 1'000 infants).
See also their article titled "Fertility in Rural Chile" (1973).
Their work also showed (p. 22 in "Nutrition and an Active Life: From Knowledge to Action" by Wilma Freire, 2005, PAHO) that bottle-fed infants who survive the first three months are three times more likely to die by age three than are breast-fed infants.
Puffer RR and Serrano CV (sic!) wrote many books, including "Patterns of Mortality in Childhood", 1973, PAHO.
See also the book "Birthweight, Maternal Age, and Birth Order: Three Important Determinants in Infant Mortality" by Ruth Rice Serrano and Carlos V. Puffer — as well as other books and articles written by these authors.
The authors list a number of publications, some of which have reached a larger audience, for example an interview in the New Internationalist in 1973 with David Morley and Ralph Hendrikse, two pediatricians who were working for change in Africa.
In 1974 a brochure titled "The Baby Killer", written by Mike Muller and published by the charitable organization War on Want in London, uncovered the shocking practices used by baby formula companies.
Additional publications, for example, a Consumer’s Union investigation into the food and pharma industries by Robert Ledogar and the book "The Nutrition Factor" by Alan Berg, prompted the WHO in 1974 to conduct a review of the practices of these multinational formula companies.
The documentary "Bottle Babies" by Peter Krieg (pseudonym), which was filmed in 1975, brought this issue into the spotlight.
Around this time, Arbeitsgruppe Dritte Welt (AgDW) (a Swiss third world action group) translated "The Baby Killer" into German. For the German version, AgDW retitled the film "Nestlé Kills Babies".
This led to a libel suit against Nestlé, which unfortunately ended up causing more harm than good. Shortly before the trial began, the formula manufacturer created the International Council of Infant Formula Industries (ICIFI) as a way to better and more neutrally influence the public. The council announced its intentions to publish a code of ethics that the formula companies would then follow.
The process set off a chain reaction in the United States: American church groups concerned with world hunger and social responsibility filed stockholder resolutions with American companies in which they owned stocks, requesting information on international sales practices
(p. 157).
After these and other steps were taken, Bristol Meyers agreed to remove its milk nurses from Jamaica. And Abbott agreed to at least not send out its “mothercraft nurses” in uniform.
In Minnesota, a consumer organization called Infant Formula Action Coalition (INFACT) was created; INFACT started a consumer boycott against Nestlé in 1977. See the box below for more information.
Senator Edward Moore Kennedy (Teddy, Ted Kennedy) was the chairman of the Subcommittee on Health and Scientific Research in 1978. In the same year, he held a hearing on the use and promotion of baby formula in developing countries. This hearing received much attention from politicians and the national media. His main question was as follows:
Can a product which requires clean water, good sanitation, adequate family income, and a literate parent to follow printed instructions, be properly and safely used in areas where water is contaminated, sewage runs in the streets, poverty is severe, and illiteracy high? (S. 159)
At this hearing, Dr. Derrick B. Jelliffe (1921–1992) described how even cans of puppy formula have a warning on them that puppies should not be given the puppy formula in the first few days of life so that they can nurse and receive colostrum from their mother. He made the point that this warning was not present on cans of formula, which would be consumed by infants.
Dr. Natividad N. Relucio Clavano (1932–2007), Chief of Pediatrics at Baguio General Hospital in the Philippines, made a statement that was even more dramatic. Her hospital had banned all formula advertisements, asked the milk nurses from the formula manufacturers to leave the hospital, and actively promoted breast-feeding. She reported on the results:
In just over four years, in a population of 10'000 infants, the breastfeeding rate jumped from 26 % to 87 % ... we were able to reduce our infant deaths by over 47 % and diseases by 58 %. Diarrhea was reduced by 79 % (p. 160).
The Kennedy hearings represent a turning point after which mothers increasingly chose to breast-feed. It also led the WHO and UNICEF to make recommendations and hold further meetings on the issue, for example, the meeting in October 1979 in Geneva titled "Infant and Young Child Feeding".
1.5 million babies died each year because they did not receive breast milk
In 1979, the WHO listed out the 50 brands and 200 varieties of breast milk substitutes. UNICEF estimated that 1.5 million babies died each year because they did not receive breast milk.

See also the book "The One Best Way?: Breastfeeding History, Politics, and Policy in Canada" by Tasnim Nathoo and Aleck Ostry (2009), who give a similar account of the work of Dr. David C. Morley (1923–2009) and Ralph Hendrikse.
In the entry "Ethics in pharmaceutical sales", Wikipedia shows how certain aspects of business ethics are often lacking in corporations. See also these beneficial anticompetitve practices.
Wikipedia has a separate entry on the Nestlé boycott.
The authors quote various passages from the book "The International Code of Marketing of Breast-Milk Substitutes" by Sami Shubber.
Jean-Claude Buffle wrote the book "Dossier N. comme Nestlé" (fr.), which was published in 1986.
However, many initiatives sponsored by Nestlé and Coca Cola followed soon thereafter, such as the International Nutrition Congress in Rio de Janeiro.
Media Benjamin, one of the participants at the conference distributed a petition criticizing the promotion of infant formula and was then promptly arrested and imprisoned. She was only released after a U.S. government agency intervened, and then she was sent back to the U.S. wearing men’s clothing as a disguise. This is a good example of the power that these corporations wield.






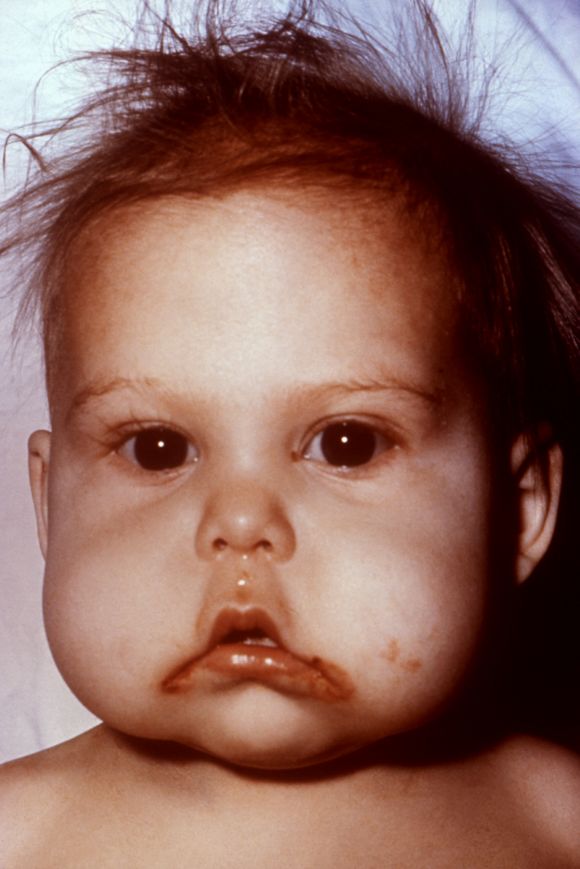
Comments